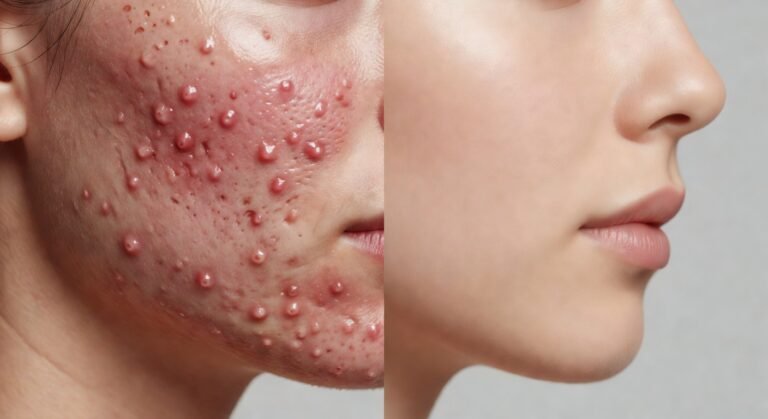
Sensitive Acne-Prone Skin: Powerful Daily Fixes
If you have sensitive acne-prone skin, you already know the maddening catch-22: the products strong enough to fight breakouts often torch your face, and the gentle stuff feels about as effective as splashing water on a grease fire. I’ve spent over a decade studying, testing, and recommending acne skincare protocols — and I can tell you that most mainstream advice completely ignores the people stuck in this overlap.
The result? Wrecked moisture barriers, chronic redness, and a medicine cabinet full of half-used bottles that each promised to be “the one.” Sound familiar? Good. You’re in the right place. I’m going to walk you through daily fixes that respect your sensitivity while genuinely clearing your skin — backed by dermatological research, not influencer hype.
If you’re brand new here, I recommend starting with my beginner’s guide for a solid foundation before we get into the advanced stuff below.
Table of Contents
- What Makes Sensitive Acne-Prone Skin So Tricky?
- The Skin Barrier: Why It’s the Real MVP
- Your Daily Sensitive Skin Routine (Step by Step)
- Ingredients to Embrace — and Ones to Ditch Immediately
- Myth-Busting: Common Lies About Acne Skincare
- Advanced Tactics for Breakout Prevention
- When to See a Dermatologist (No Shame in It)
- FAQ: Sensitive Acne-Prone Skin
- My Top Recommended Gear
What Makes Sensitive Acne-Prone Skin So Tricky?
Sensitive acne-prone skin occurs when a compromised or reactive skin barrier coexists with overactive sebaceous glands and a tendency toward inflammatory breakouts. Managing it requires balancing acne treatment with gentle skincare to avoid triggering redness, burning, or further barrier damage — a challenge that standard acne protocols rarely address.
Here’s what most people get wrong: they treat acne and sensitivity as two separate problems. They’re not. They’re deeply interconnected, and treating one while ignoring the other is why so many routines fail catastrophically.
Your skin has a built-in defense system — the acid mantle and lipid barrier — that keeps irritants out and moisture in. When acne shows up, the instinct (fueled by decades of marketing garbage) is to strip, scrub, and nuke everything. But aggressive acne treatment tips destroy the very barrier that keeps your skin calm. The result? Your skin overproduces oil to compensate, inflammation spikes, and you break out even worse. It’s a vicious cycle, and I’ve watched hundreds of people spin in it for years.
According to research published by the National Institutes of Health (NIH), approximately 60-70% of people with acne also report skin sensitivity, suggesting significant overlap between these conditions. This isn’t a rare combo — it’s arguably the norm.
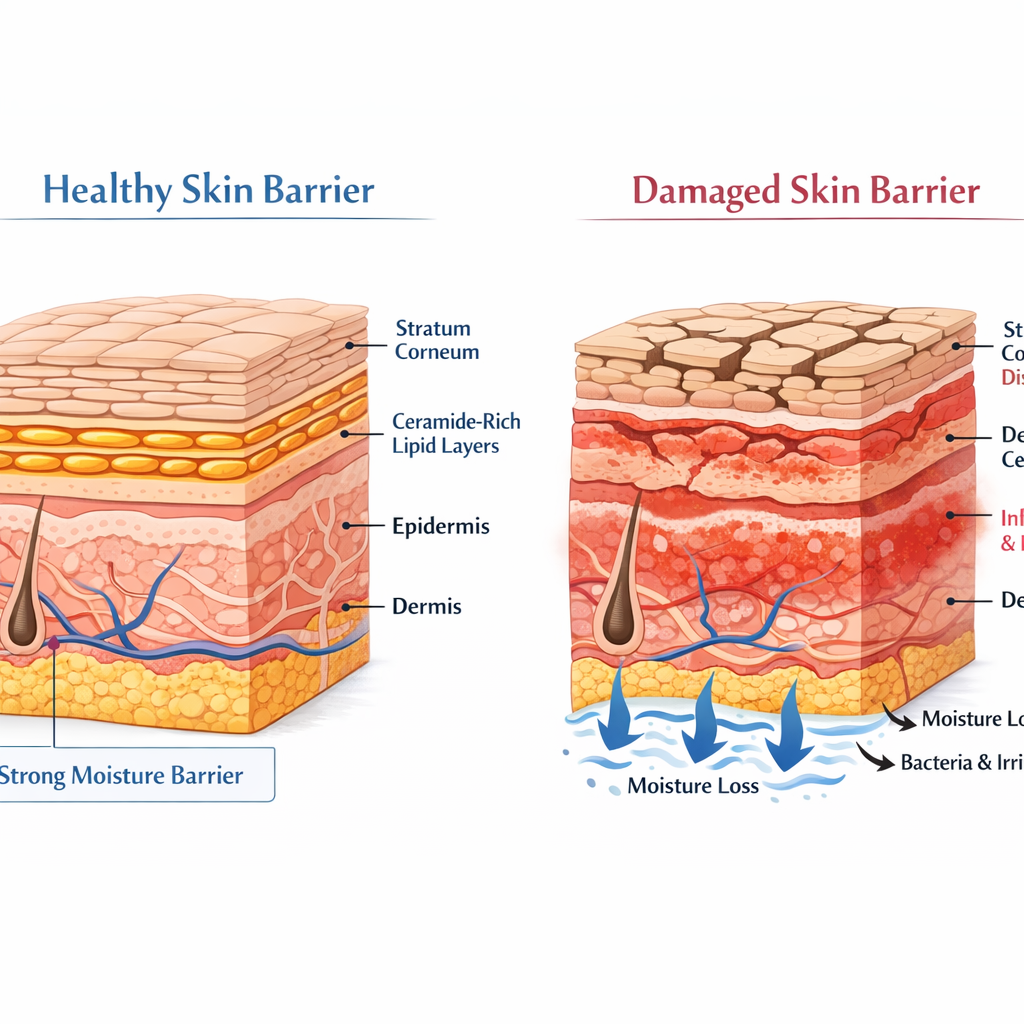
The Skin Barrier: Why It’s the Real MVP
I can’t stress this enough: skin barrier repair is not a trendy buzzword — it’s the single most important concept for anyone dealing with reactive, breakout-prone skin. Think of your barrier like the bouncer at a club. When it’s strong, it decides what gets in and what stays out. When it’s wrecked, everything rushes in — bacteria, pollutants, allergens — and your skin panics.
Signs Your Barrier Is Compromised
- Stinging or burning when you apply products (even “gentle” ones)
- Tightness after cleansing that won’t go away
- Patches of dryness alongside oily, acne-prone zones
- Redness that seems constant, not just post-breakout
- Products that used to work suddenly irritate you
If you’re nodding along to three or more of those, your barrier needs attention before you add any active acne-fighting ingredients. I know that feels counterintuitive when you’ve got active breakouts, but trust me — and trust the research from the American Academy of Dermatology — a repaired barrier responds dramatically better to treatment.
To understand the different types of breakouts you might be dealing with alongside sensitivity, check out my acne types breakdown. Knowing what you’re fighting changes how you fight it.
Your Daily Sensitive Skin Routine (Step by Step)
Here’s the sensitive skin routine framework I recommend. It’s not a 12-step K-beauty marathon — it’s streamlined, strategic, and designed to calm your skin while quietly tackling breakouts in the background. IMO, simplicity wins every time with reactive skin.
Morning Routine
- Step 1 — Gentle Cleanser: Use a fragrance-free, low-pH (5.0–5.5) gel or cream cleanser. Avoid foaming sulfate-based washes. I prefer ceramide-containing formulas that clean without stripping.
- Step 2 — Hydrating Toner or Essence: A light layer of something with hyaluronic acid or centella asiatica to prep the skin. Skip anything with alcohol or witch hazel.
- Step 3 — Niacinamide Serum (2%–5%): This is your multitasker. It reduces sebum production, calms inflammation, and supports barrier function. Higher concentrations (10%+) can irritate sensitive types — stay moderate.
- Step 4 — Moisturizer: Non-comedogenic, ceramide-rich, fragrance-free. Period.
- Step 5 — Mineral Sunscreen: Zinc oxide or titanium dioxide, SPF 30+. Chemical filters like oxybenzone can trigger sensitivity flares.
Evening Routine
- Step 1 — Double Cleanse: Oil-based cleanser first (to dissolve sunscreen and sebum), followed by your gentle water-based cleanser.
- Step 2 — Active Treatment (alternating nights): Adapalene 0.1% (OTC as Differin) or a low-percentage salicylic acid (0.5%–1%). Apply every other night to start. Use the “sandwich method” — moisturizer, then active, then moisturizer — to buffer irritation.
- Step 3 — Moisturizer: Same as morning. Layer it generously at night.
- Step 4 — Occlusive (optional): A thin layer of petroleum jelly or squalane oil on dry patches locks everything in.
For a deeper look at treatment options that work alongside this routine, explore my full acne treatments resource.

Ingredients to Embrace — and Ones to Ditch Immediately
I’ve learned this the hard way (and so have many of my readers): ingredient literacy separates people who clear their skin from people who chase their tails for years. Here’s my no-BS cheat sheet for gentle skincare that actually fights acne.
Green Light Ingredients
- Niacinamide (Vitamin B3): Anti-inflammatory, sebum-regulating, barrier-supporting. The Swiss Army knife of sensitive acne care.
- Centella Asiatica (Cica): Proven wound-healing and anti-redness properties. Your skin loves this stuff.
- Ceramides: The literal building blocks of your barrier. Non-negotiable.
- Azelaic Acid (10%–15%): Kills acne bacteria, reduces hyperpigmentation, and is remarkably well-tolerated by sensitive skin. Honestly underrated.
- Adapalene (0.1%): The only retinoid I’d recommend for most sensitive-skin beginners. The FDA approved it for OTC use, and clinical data supports its efficacy with a gentler irritation profile than tretinoin.
Red Flag Ingredients
- Fragrance (Parfum): Top sensitizer. Adds nothing therapeutic. Ditch it.
- Denatured Alcohol (Alcohol Denat.): Strips lipids, destroys barrier function.
- Sodium Lauryl Sulfate (SLS): Harsh surfactant common in foaming washes. Swap for sodium lauroyl sarcosinate or cocamidopropyl betaine.
- Essential Oils: Tea tree, lavender, peppermint — they all carry sensitization risk. “Natural” does not mean “safe for sensitive skin.”
- High-Concentration Glycolic Acid: AHAs above 5% can be too aggressive. If you need exfoliation, BHA (salicylic acid) or PHAs are smarter choices because they’re less irritating.
Myth-Busting: Common Lies About Acne Skincare
After a decade in this space, these myths still make me twitch. Let me set the record straight on the biggest offenders.
Myth #1: “You need to dry out your acne.”
Wrong. Dehydrating your skin triggers compensatory oil production and barrier breakdown. Hydrated skin heals faster and responds better to treatment. Period.
Myth #2: “If a product stings, it’s working.”
Absolutely not. Stinging means your barrier is compromised and the product is causing damage, not delivering results. Clear skin tips from the 1990s need to stay there.
Myth #3: “Oily skin doesn’t need moisturizer.”
This one kills me. Every skin type needs moisturizer. Skipping it on oily, acne-prone skin worsens dehydration and increases breakouts. Use a lightweight gel formula if full creams feel heavy.
Myth #4: “Sunscreen causes acne.”
Bad sunscreen causes acne. The right mineral sunscreen — non-comedogenic, fragrance-free — protects against UV-induced inflammation and post-acne dark marks. Stop blaming the category and start reading labels.
If you’re dealing with additional concerns beyond breakouts, like scarring or hyperpigmentation, my skin concerns hub covers those in depth.
Advanced Tactics for Breakout Prevention
You’ve got the basics down. Now let me share the strategies that separate good results from great results — the insider-level breakout prevention tactics I’ve refined over years of working with reactive skin.
1. Contact Therapy (Short Contact Time)
Can’t tolerate leave-on benzoyl peroxide or salicylic acid? Apply it to clean skin, wait 5–10 minutes, then rinse it off. You get approximately 60–70% of the antibacterial benefit with a fraction of the irritation. Dermatologists have used this approach for decades, yet it barely gets mentioned online. You’re welcome 🙂
2. Strategic Spot Treatment Rotation
Don’t use the same active everywhere every night. Apply adapalene to your chronic breakout zones (chin, jawline) and skip it on reactive areas (cheeks, around the nose). Your face isn’t one uniform surface — stop treating it like one.
3. Pillow Hygiene Protocol
Change your pillowcase every 2–3 days. Use silk or satin — they create less friction and harbor fewer bacteria than cotton. This is one of the simplest clear skin tips I give, and people consistently underestimate its impact.
4. Monitor Hormonal Patterns
Track your breakouts against your menstrual cycle (if applicable). Hormonal acne follows predictable patterns, and timing your strongest actives to pre-breakout windows dramatically improves outcomes. My guide on adult acne in women covers this strategy extensively.
Expert Commentary: This video from a board-certified dermatologist breaks down the essentials of building a sensitive-skin-safe acne routine — I recommend it because it reinforces the barrier-first philosophy with real clinical reasoning, not just product pushing.
When to See a Dermatologist (No Shame in It)
Look, I’m all about empowering people with knowledge — but I also know when to say “this is above your pay grade.” See a dermatologist if:
- Your acne is cystic or nodular (deep, painful bumps that don’t surface)
- Over-the-counter treatments haven’t improved things after 8–12 consistent weeks
- You’re developing significant scarring
- Your sensitivity is so severe that even the gentlest products cause reactions
- You suspect a hormonal component (irregular periods, jawline-dominant breakouts)
A derm can prescribe tools you simply can’t access OTC — spironolactone, prescription-strength azelaic acid, oral antibiotics for acute flares, or isotretinoin for severe cases. The National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) maintains excellent patient resources on when professional intervention makes sense. There’s zero weakness in getting expert help — it’s actually the smartest move you can make tbh.

FAQ: Sensitive Acne-Prone Skin
What is the best moisturizer for sensitive acne-prone skin?
The best moisturizer for sensitive acne-prone skin is a fragrance-free, non-comedogenic formula containing ceramides, niacinamide, or hyaluronic acid. These ingredients hydrate and support skin barrier repair without clogging pores or triggering breakouts.
Can I use retinol on sensitive acne-prone skin?
Yes, but start with a low-concentration retinol (0.025%–0.03%) and apply it every third night, gradually increasing frequency. Buffer it over moisturizer to reduce irritation. Prescription retinoids like adapalene are also well-tolerated by many sensitive skin types.
How often should I exfoliate sensitive acne-prone skin?
Limit chemical exfoliation to 1–2 times per week using a gentle BHA (salicylic acid at 0.5%–2%) or a PHA (polyhydroxy acid). Avoid physical scrubs, as they can micro-tear sensitive skin and worsen inflammation and breakouts.
Does diet affect sensitive acne-prone skin?
Research from the American Academy of Dermatology suggests high-glycemic foods and dairy may worsen acne in some individuals. While diet alone won’t cure acne, reducing processed sugars and prioritizing anti-inflammatory foods can support clearer skin alongside a proper sensitive skin routine.
Should I skip sunscreen if it breaks me out?
Never skip sunscreen. Instead, switch to a mineral-based (zinc oxide or titanium dioxide) sunscreen labeled non-comedogenic and fragrance-free. UV damage worsens post-inflammatory hyperpigmentation and weakens the skin barrier, making acne skincare harder to manage long-term.
My Top Recommended Gear
These are products I’ve either personally used, recommended to readers, or vetted through ingredient analysis. They align with every principle I’ve outlined above — gentle, effective, and formulated for reactive, breakout-prone skin.
- CeraVe Foaming Facial Cleanser (Sensitive Skin): A ceramide-rich, fragrance-free cleanser that removes excess oil without destroying your barrier. Check price on Amazon
- La Roche-Posay Toleriane Double Repair Moisturizer: Niacinamide + ceramides + prebiotic thermal water. Non-comedogenic, fragrance-free, and genuinely calming. Check price on Amazon
- EltaMD UV Clear Broad-Spectrum SPF 46: The gold standard mineral sunscreen for acne-prone skin. Contains niacinamide and zinc oxide. Dermatologist-recommended for good reason. Check price on Amazon
Disclaimer: This post contains affiliate links. As an Amazon Associate, I may earn a commission from qualifying purchases at no additional cost to you.