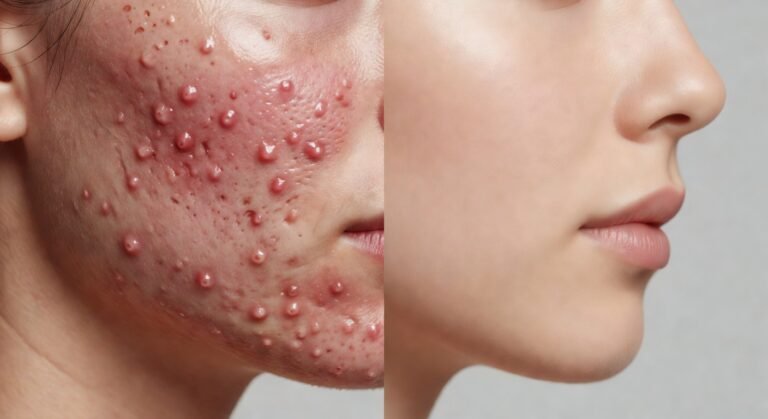
Comedonal Acne: Simple Habits That Change Skin
If cystic acne is the fire alarm, comedonal acne is the smoldering wiring inside the wall — silent, invisible, and absolutely devastating when ignored. Most people obsess over the big angry pimples and completely ignore the army of blackheads and whiteheads quietly preparing a full-scale invasion of their face. That’s the problem. The agitation? Those tiny clogged pores don’t just stay tiny. Left unchecked, they escalate into inflamed nodules, post-inflammatory hyperpigmentation, and the kind of scarring that makes you feel like your skin is working against you. The solution, thankfully, is not complicated — but it does require you to stop doing what doesn’t work and start doing what actually moves the needle.
Table of Contents
- What Is Comedonal Acne, Exactly?
- Blackheads vs. Whiteheads: Stop Confusing Them
- The Daily Habits That Are Silently Clogging Your Pores
- Building a Skincare Routine That Actually Works
- The Ingredients Worth Your Money (and the Ones That Aren’t)
- When Comedonal Acne Escalates to Cystic Acne
- Advanced Tactics Most People Overlook
- Frequently Asked Questions
- My Top Recommended Gear
What Is Comedonal Acne, Exactly?
Quick Answer: Comedonal acne is a non-inflammatory form of acne caused by follicles plugged with excess sebum and dead skin cells. It manifests as blackheads (open comedones) and whiteheads (closed comedones) and commonly affects the forehead, nose, and chin. It’s not infected — but it can become infected if you ignore it.
I’ve spent over a decade digging through clinical research, product formulations, and the messy reality of acne-prone skin. What I’m sharing here isn’t recycled Pinterest advice. This is the real playbook — habits, ingredients, and mindset shifts that produce genuine, measurable skin improvement.
Comedones form when your sebaceous glands produce more oil than your skin can handle, and that oil mixes with dead skin cells to form a plug inside a hair follicle. The National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) confirms that this process is the foundational event in all acne — every pustule, nodule, and cyst you’ve ever had started as a comedone.
Here’s what makes comedonal acne unique: it’s largely non-inflammatory. There’s no significant bacterial invasion yet, no immune system freak-out. You’re dealing with a plumbing problem, not an infection. That distinction completely changes how you treat it. Want to understand how comedonal acne fits into the broader acne spectrum? This breakdown of acne types gives you the full picture.
Blackheads vs. Whiteheads: Stop Confusing Them
I see this mixed up constantly, and the confusion leads people to use the wrong treatments. So let me make this crystal clear:
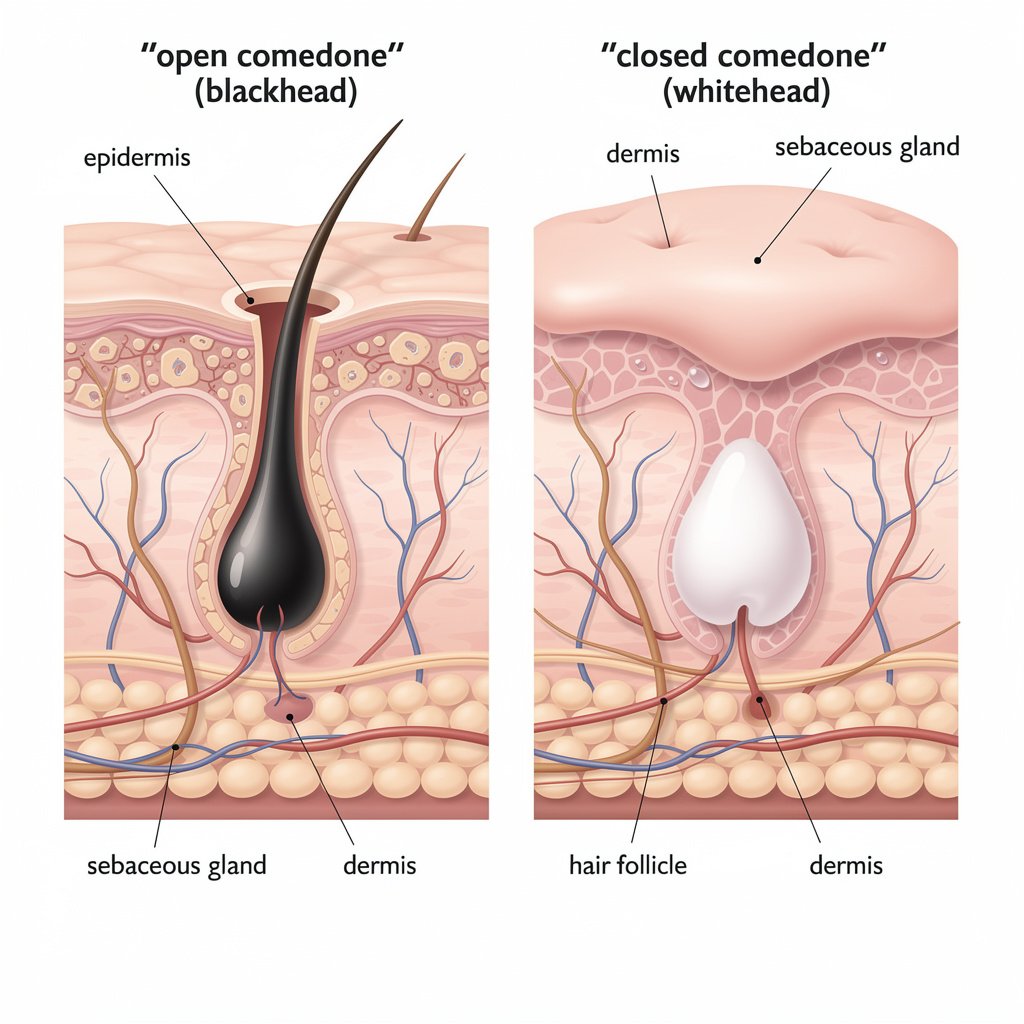
- Blackheads (open comedones): The follicle is open at the surface. The plug oxidizes when exposed to air — that’s why it looks black or dark brown. It has nothing to do with dirt. Scrubbing your face like you’re sanding a deck will not fix this.
- Whiteheads (closed comedones): The follicle opening is sealed over by a thin layer of skin. No oxidation occurs, so it appears white or skin-colored. These are often harder to treat because the active ingredient needs to penetrate that skin barrier to reach the plug.
Why does this distinction matter? Because your treatment approach shifts. Blackheads respond well to exfoliating acids — particularly BHA (salicylic acid) — which can penetrate oil and dissolve the plug. Whiteheads need that plus something to accelerate cell turnover, which puts retinoids front and center.
The Daily Habits That Are Silently Clogging Your Pores
Here’s where I get to say something most skincare content won’t: your problem probably isn’t your genetics. It’s your routine. The habits below are the most common offenders I’ve seen sabotage otherwise solid skincare efforts:
1. Over-Washing Your Face
Washing twice a day? Smart. Three, four, five times? You’re stripping your skin’s natural barrier, triggering a compensatory sebum surge, and making your clogged pores significantly worse. Once in the morning and once at night is the clinical sweet spot — and if you wear heavy sunscreen or makeup, double-cleansing at night is legitimate and effective.
2. Using Comedogenic Products
The term “non-comedogenic” on a label is marketing, not law — there’s no FDA regulation mandating that companies prove this claim. I check the comedogenicity ratings of specific ingredients before recommending any product to acne-prone skin. Common offenders hiding in “clean” or “natural” products include coconut oil, cocoa butter, and isopropyl myristate.
3. Skipping Sunscreen (or Using the Wrong One)
Skipping SPF causes UV-induced inflammation that worsens acne and accelerates post-acne dark marks. But using a thick, occlusive sunscreen on acne-prone skin is equally counterproductive. I recommend lightweight, mineral-based or hybrid formulas — specifically those containing zinc oxide, which also carries mild anti-inflammatory and antimicrobial properties. If you’re not sure where to start with your overall approach, this beginner’s guide walks you through the foundational steps.
4. Touching Your Face Constantly
Your hands carry sebum, bacteria, and environmental debris. Every time you rest your chin on your hand or pick at a whitehead, you transfer that material directly into an already-compromised follicle. IMO, this single habit change — just stopping the face touching — produces noticeable improvement within two weeks for most people.
5. Ignoring Pillowcases and Phone Screens
Your pillowcase accumulates oil, dead skin cells, and product residue every single night. Your phone screen contacts your cheek for hours a day. Change your pillowcase 2–3 times per week and wipe your phone screen daily. These are boring tips, but they make a real difference.
Building a Skincare Routine That Actually Works
A solid skincare routine for acne-prone skin doesn’t need to be a 12-step production. In fact, complexity is usually the enemy of clear skin — more products mean more potential irritants, more comedogenic ingredients, and more chances to disrupt your skin barrier. Here’s the framework I use:
Morning Routine
- Gentle cleanser — Avoid anything with sulfates or fragrance. A pH-balanced gel cleanser is ideal.
- Lightweight moisturizer — Yes, even oily, acne-prone skin needs moisture. Dehydrated skin overproduces sebum. Use something with niacinamide — it’s anti-inflammatory and regulates oil production.
- Mineral SPF 30+ — Every single day. No exceptions. Rain, indoors, winter — still yes.
Evening Routine
- Double cleanse (if you wore SPF or makeup) — Oil cleanser first, then water-based cleanser.
- BHA exfoliant (2–3 nights per week) — Salicylic acid 1–2% penetrates the follicle and dissolves the comedone plug from the inside out.
- Retinoid (alternate nights) — Retinol or prescription tretinoin accelerates cell turnover, preventing dead skin cell buildup. Start low and slow to avoid purging that derails your consistency.
- Moisturizer — Applied after retinoid to buffer irritation without negating efficacy.
For deeper guidance on which treatments fit which acne type and severity, this comprehensive acne treatments resource breaks down prescription, OTC, and professional options side by side.

The Ingredients Worth Your Money (and the Ones That Aren’t)
The skincare industry generates billions by convincing you that exotic ingredients in $200 serums will fix your skin. I’m here to save you money. The clinical evidence base for acne treatment (via the NIH National Library of Medicine) consistently points to the same core actives — most of which are dirt cheap:
- Salicylic Acid (BHA): Oil-soluble, penetrates follicles, anti-inflammatory. The gold standard for blackhead and whitehead removal. Effective at 0.5–2%.
- Retinoids (Retinol / Tretinoin): The most well-researched anti-acne, anti-aging class of ingredients in existence. Tretinoin (prescription) outperforms OTC retinol, but both work. Consistency matters more than concentration.
- Niacinamide: Reduces sebum production, strengthens the skin barrier, fades post-acne marks. Works synergistically with everything else on this list.
- Benzoyl Peroxide: More useful for inflammatory acne than comedonal, but a low-concentration leave-on (2.5%) can prevent comedones from getting infected.
- Azelaic Acid: Underrated. Anti-inflammatory, anti-comedonal, and effective for hyperpigmentation. Available OTC at 10% and prescription at 15–20%.
What to skip: Most toners with alcohol, physical scrubs with large or irregular particles (they cause micro-tears and worsen inflammation), and anything with fragrance if your skin barrier is already compromised.
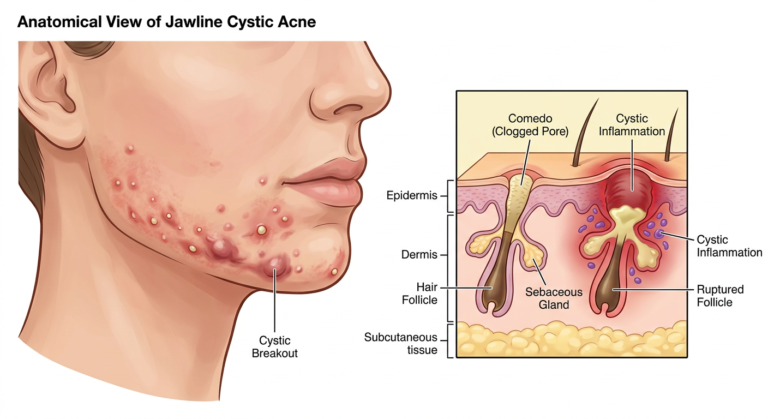
When Comedonal Acne Escalates to Cystic Acne
This is the part nobody wants to read, but you need to hear it. Comedones don’t stay comedones forever if you ignore them. Cutibacterium acnes (C. acnes), the bacterium that lives in your follicles, feeds on sebum. When a comedone creates an anaerobic (oxygen-free) environment with a buffet of sebum, C. acnes multiplies rapidly and triggers an immune response. That inflammation drives the lesion deeper into the dermis — and suddenly you have a nodule or cyst instead of a whitehead.
Cystic acne is a different beast altogether — painful, deep, and prone to permanent scarring. If you’re already dealing with it, don’t try to manage it solo. A dermatologist can prescribe isotretinoin, oral antibiotics, or intralesional corticosteroid injections that produce results OTC products simply cannot match. I’ve written extensively about this progression at the cystic acne hub — it’s worth a read if you’re seeing deep, painful lesions.
Also worth considering: hormonal fluctuations dramatically accelerate comedone formation and the escalation to inflammatory acne. If your breakouts follow a monthly pattern or cluster around the jawline, hormonal acne deserves serious attention. The American Academy of Dermatology confirms that hormonal factors play a significant role in adult acne, particularly in women over 25.
Advanced Tactics Most People Overlook
You’ve got the basics down. Now let’s talk about the moves that separate a solid routine from a genuinely optimized one.
Skin Cycling
Skin cycling — popularized in dermatology circles and then taken viral on social media — is the practice of rotating actives across a 4-night cycle: exfoliant night, retinoid night, recovery night, recovery night. This approach lets you use strong actives without compounding irritation. If you’re experiencing barrier disruption from your current routine, adopting this cycle often resolves it within two weeks. 🙂
Dietary Influence Is Real (But Overstated)
The dairy-acne link has actual research behind it — particularly skim milk, which contains whey proteins that spike IGF-1 (a hormone that boosts sebum production). High-glycemic foods similarly trigger insulin spikes that upregulate androgen activity. Does this mean you need to become a dairy-free, sugar-free monk? No. But if your skin is chronically resistant to topical treatment, your diet deserves an honest audit. Reducing processed sugar and dairy for 8 weeks is a zero-risk experiment worth trying.
Professional Treatments Worth the Investment
- Chemical peels (salicylic or glycolic): A professional-grade exfoliation session can clear a backlog of comedones faster than weeks of home treatment.
- Comedone extraction by an esthetician: Properly done, manual extraction clears existing comedones without spreading bacteria. DIY pore strips and fingers at home? That’s how you create inflammation and scarring.
- Blue light therapy: Targets C. acnes bacteria directly. Useful as an adjunct — not a standalone treatment — for preventing comedonal escalation.
For a curated look at which products actually deliver results at every price point, check out these independent product reviews — I’ve done the legwork so you don’t have to spend money on duds.
Expert Commentary: This video delivers a board-certified dermatologist’s clinical walk-through of comedone formation and treatment hierarchy — exactly the kind of authoritative, no-hype explanation that puts your DIY research in proper medical context.
The Myth of “Purging” as an Excuse
Let me bust a myth that I see weaponized to justify bad products: purging is real, but it’s specific. Purging — the temporary increase in breakouts when starting a new active — only happens with ingredients that accelerate cell turnover (retinoids, AHAs, BHAs). It appears in areas where you already break out, and it resolves within 4–6 weeks. If a new moisturizer or sunscreen is causing breakouts in new areas after 6+ weeks, that’s not purging — that’s a comedogenic product breaking you out. Stop using it.
Frequently Asked Questions
What is the difference between comedonal acne and cystic acne?
Comedonal acne involves non-inflammatory blocked follicles — blackheads and whiteheads — that sit near the skin’s surface. Cystic acne is a severe, inflammatory form that develops deep beneath the skin, causing painful, fluid-filled nodules that often leave scars. TBH, if you’re dealing with cysts, please see a dermatologist — OTC products have real limits here.
Can comedonal acne turn into cystic acne?
Yes. If you leave comedones untreated, bacteria (C. acnes) can colonize the clogged follicle, trigger an immune response, and push the lesion deeper — resulting in nodules or cysts. Early treatment of comedones is your best prevention strategy.
How long does it take for comedonal acne to clear?
With a consistent skincare routine using proven actives like retinoids and salicylic acid, most people see meaningful improvement in 8–12 weeks. Skin cell turnover takes time — patience is non-negotiable. Anyone promising faster results is selling you something.
Is comedonal acne hormonal?
It can be. Androgens stimulate sebaceous glands to produce excess sebum, which feeds comedone formation. If your breakouts cluster around the jawline or chin and flare cyclically, hormones are likely a major driver — and that calls for a different treatment approach than topical-only management.
My Top Recommended Gear
These are the product categories I consistently recommend for managing comedonal and acne-prone skin. I’ve linked each to current options on Amazon so you can compare formulas and reviews yourself:
- Salicylic Acid BHA Exfoliant: The cornerstone of any comedone-clearing routine. Look for a leave-on formula at 2%.
Browse Salicylic Acid BHA Exfoliants on Amazon → - Retinol Serum for Acne-Prone Skin: Accelerates cell turnover and prevents the dead skin buildup that feeds comedone formation. Start at 0.25–0.5% if you’re new to retinoids.
Browse Retinol Serums on Amazon → - Mineral Sunscreen SPF 30+ for Oily Skin: Non-negotiable daily step — protect your skin and prevent dark marks from worsening.
Browse Mineral Sunscreens on Amazon →
Disclaimer: This post contains affiliate links. As an Amazon Associate, I may earn a commission from qualifying purchases at no additional cost to you. All product recommendations are based on independent research and genuine editorial judgment — affiliate relationships do not influence my assessments.