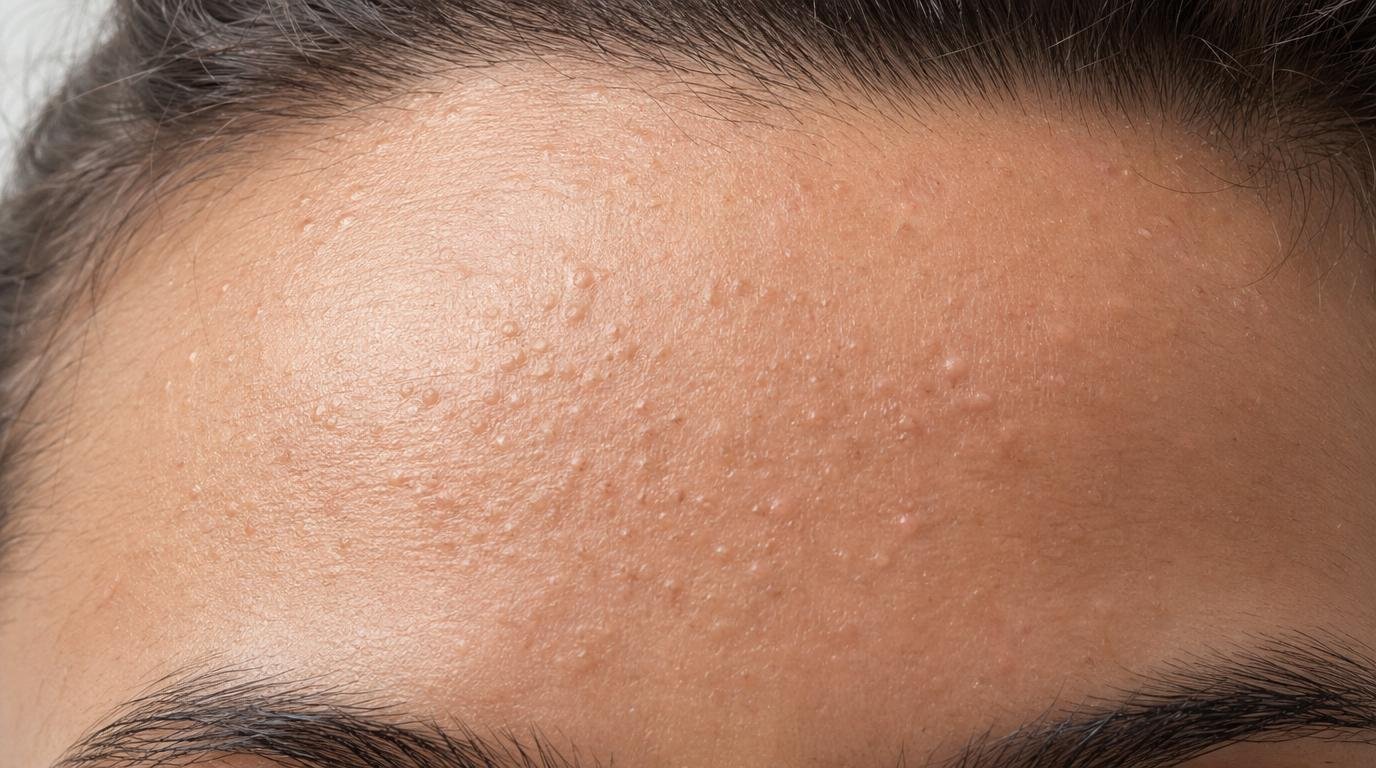
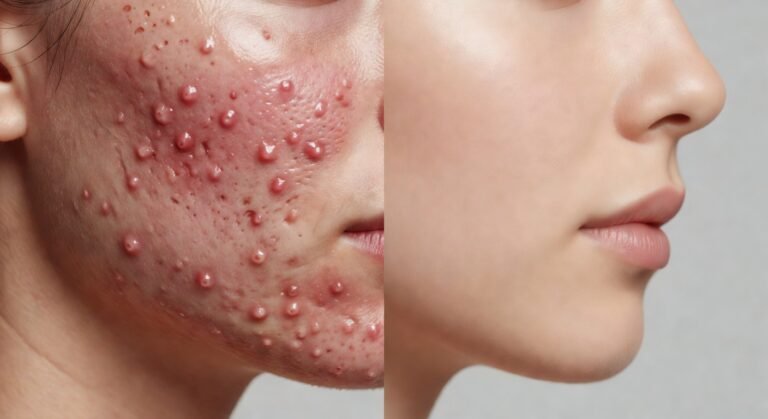
Fungal Acne on Forehead: 7 Warning Signs to Know
Fungal acne on forehead is often mistaken for regular acne — but the treatment approach is completely different.
You’ve been battling fungal acne on your forehead for months. You’ve tried every cleanser, every spot treatment, every “miracle” product. Nothing works. In fact, some things seem to make it worse.
Here’s the painful truth: you might be treating the wrong thing entirely. Most people — and even some well-meaning skincare routines — mistake fungal acne for regular bacterial acne. But these two conditions need completely different treatments.
Using the wrong treatment doesn’t just fail to help. It can actively make fungal acne spread and multiply. I’ve seen this pattern over and over again. The good news? Once you correctly identify fungal acne, it’s very treatable. Let me show you exactly how to spot it.
📋 Table of Contents
- What Is Fungal Acne, Exactly?
- Warning Sign #1: Your Bumps Are All the Same Size
- Warning Sign #2: It Itches More Than It Hurts
- Warning Sign #3: Regular Acne Products Make It Worse
- Warning Sign #4: You Sweat a Lot Around Your Forehead
- Warning Sign #5: You’ve Recently Used Antibiotics
- Warning Sign #6: The Bumps Cluster in One Specific Zone
- Warning Sign #7: Your Skincare Routine Is Full of Oils
- How to Actually Treat Fungal Acne on Your Forehead
- Frequently Asked Questions
- My Top Recommended Gear
What Is Fungal Acne, Exactly?
Quick Answer: Fungal acne (technically called Malassezia folliculitis) is a skin condition caused by an overgrowth of Malassezia yeast in your hair follicles. It looks like acne but is not caused by bacteria. It requires antifungal treatment, not traditional acne products. It commonly appears on the forehead, chest, and back.
Fungal acne isn’t really acne at all. The medical name is Malassezia folliculitis. It happens when a type of yeast called Malassezia overgrows inside your hair follicles.
Malassezia naturally lives on every person’s skin. It’s completely normal. The problem starts when conditions allow it to grow out of control. When that happens, it inflames your follicles and creates those frustrating bumps.
According to the National Institutes of Health, Malassezia species are involved in a range of skin conditions, including folliculitis and seborrheic dermatitis. This yeast thrives in warm, oily, and humid environments — exactly the kind of environment your forehead creates after a workout or a long day.
If you’re not sure what type of acne you’re dealing with, start here: understanding the different types of acne is the single most important first step to clearing your skin.
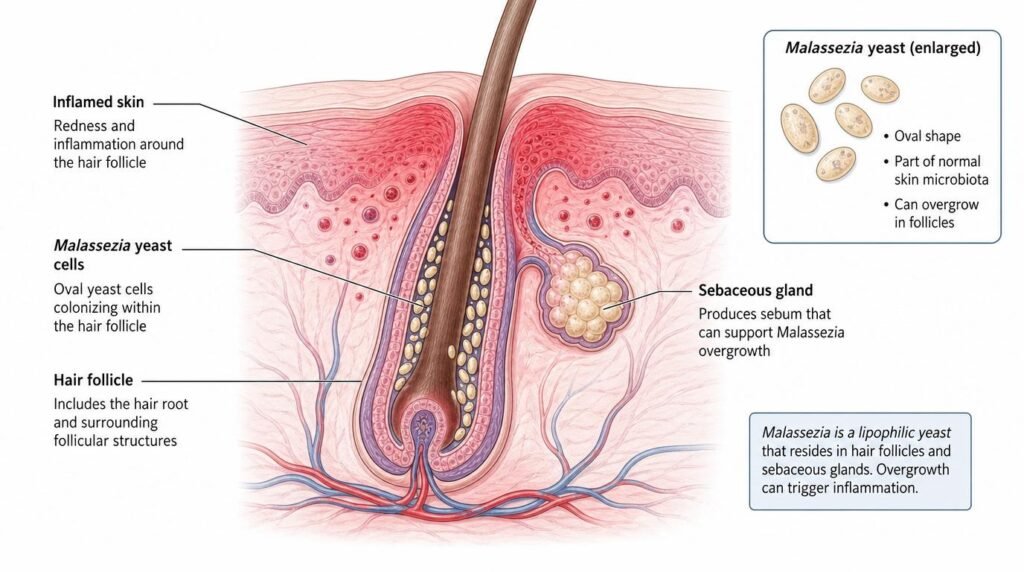
Malassezia yeast lives naturally on the skin — but overgrowth triggers fungal acne.
Warning Sign #1: Your Bumps Are All the Same Size
🚨 Key Sign: Uniform, same-size bumps on your forehead are a major red flag for fungal acne.
Regular acne is messy and unpredictable. You get whiteheads, blackheads, big cysts, tiny pimples — all mixed together. Fungal acne doesn’t work that way.
With Malassezia acne, the bumps tend to be remarkably uniform. They’re usually 1–2 mm in diameter. They look almost identical to each other, like tiny dots stamped in a pattern.
Dermatologists use this visual consistency as a strong diagnostic clue. If your forehead bumps all look the same size and shape, fungal acne should be on your radar immediately.
Warning Sign #2: It Itches More Than It Hurts
🚨 Key Sign: Itchy forehead bumps — not painful ones — point strongly toward fungal acne.
Bacterial acne is often tender or painful to touch, especially inflammatory forms like cysts or nodules. Fungal acne behaves differently.
Most people with fungal acne describe their forehead bumps as itchy. Sometimes mildly itchy. Sometimes intensely itchy. The itch gets worse with sweat or heat.
If you catch yourself scratching your forehead absentmindedly — especially after a workout or in hot weather — that itch is a sign worth paying attention to. This symptom alone won’t confirm the diagnosis, but combined with other signs, it builds a very clear picture.
People with sensitive acne-prone skin often misread this itch as a reaction to their skincare products. Sometimes it is. But often, it’s fungal acne quietly waving at you.
Warning Sign #3: Regular Acne Products Make It Worse
🚨 Key Sign: If benzoyl peroxide and salicylic acid aren’t helping (or are making things worse), reconsider the diagnosis.
This is the most telling sign I see people overlook. They buy every popular acne product. They follow every routine they see on social media. Nothing improves.
Here’s why: standard acne treatments target bacteria. Fungal acne is caused by yeast. Antibacterial ingredients simply don’t touch the root problem. Some products — especially those containing fatty acids and certain oils — actually feed Malassezia and make fungal acne spread faster.
A report from the American Academy of Dermatology emphasizes that misdiagnosed acne is one of the leading reasons treatments fail. If your current routine isn’t working after 6–8 weeks, something is wrong with the diagnosis, not just the products.
Warning Sign #4: You Sweat a Lot Around Your Forehead
🚨 Key Sign: Regular sweating or heat exposure on the forehead creates the perfect environment for Malassezia overgrowth.
Think about your lifestyle for a moment. Do you work out regularly? Wear a hat or helmet? Live in a hot, humid climate? Work a job where you sweat a lot?
Malassezia yeast loves heat and moisture. Your forehead is already one of the oiliest parts of your face. Add consistent sweat to that equation and you’ve built a perfect breeding ground.
I talk to teens who play sports every day and wonder why their forehead won’t clear up. I talk to adults who wear helmets for their commute with the same frustration. The connection between sweat, heat, and fungal acne triggers is real and well-documented.
If you’re a teenager dealing with persistent forehead bumps, I’d strongly recommend reading about teen acne and its unique triggers — fungal acne in teens is more common than most people realize.

Sweat, heat, and humidity are primary triggers for Malassezia overgrowth on the forehead.
Warning Sign #5: You’ve Recently Used Antibiotics
🚨 Key Sign: Antibiotic use — especially oral antibiotics for acne — can disrupt your skin’s microbiome and trigger fungal overgrowth.
Here’s an ironic twist. Many people take antibiotics to treat regular acne. Those antibiotics kill bacteria — including the bacteria that naturally compete with yeast on your skin.
When the bacterial competition disappears, Malassezia yeast seizes the opportunity and grows unchecked. The result? A new outbreak of bumps on the forehead — but this time, it’s fungal, not bacterial.
Research published in the Journal of Clinical and Aesthetic Dermatology confirms that antibiotic-induced dysbiosis of the skin microbiome is a recognized trigger for Malassezia folliculitis. If your “acne” appeared or worsened after a course of antibiotics, this is a crucial clue.
Warning Sign #6: The Bumps Cluster in One Specific Zone
🚨 Key Sign: Fungal acne tends to cluster — often along the hairline, across the forehead, or in distinct patches.
Regular acne appears randomly across the face. It might pop up on your chin, your cheeks, your nose. Fungal acne has a different pattern.
On the forehead, Malassezia folliculitis often clusters right along the hairline. It can also appear in bands across the mid-forehead or in dense patches where sweat and oil concentrate most.
That clustering behavior mirrors where yeast conditions are most favorable. More oil, more warmth, more occlusion — more fungal acne. If your bumps seem to “stay in their lane” rather than spreading randomly, pay attention to that pattern.
Women experiencing hormonal shifts sometimes misidentify this clustering as hormonal acne. If you’re dealing with persistent forehead bumps as an adult woman, it’s worth exploring adult acne in women and how to differentiate the causes before committing to any treatment.
Warning Sign #7: Your Skincare Routine Is Full of Oils
🚨 Key Sign: Certain fatty acids and oils — including many “natural” and “skin-loving” ingredients — directly feed Malassezia yeast.
This one stings a little because the natural skincare world loves its oils. Rosehip oil. Argan oil. Coconut oil. Squalane. They sound beautiful. But many of these contain the exact fatty acids that Malassezia needs to thrive.
According to research on Malassezia lipid dependency from PubMed Central, these yeasts are lipid-dependent organisms. They literally consume fatty acids. Slathering your forehead in oil-rich products creates a buffet for fungal acne.
Check your moisturizer. Check your sunscreen. Check your serum. Look for ingredients like lauric acid, oleic acid, myristic acid, and linoleic acid. These are common feeding grounds for Malassezia. Switching to a fungal acne-safe routine often produces dramatic improvements within weeks.
💡 Pro Tip: The website Skin Smart maintains a free database where you can check if your skincare products are safe for fungal acne. A 5-minute audit of your current routine could change everything.
How to Actually Treat Fungal Acne on Your Forehead
Now that you’ve identified the signs, let’s talk about what actually works. Treatment for fungal acne on the forehead is straightforward once you know what you’re fighting.
Step 1: Switch to an Antifungal Cleanser
Look for a cleanser containing ketoconazole or selenium sulfide. These are proven antifungal agents. Use the cleanser on your forehead, let it sit for 60–90 seconds, then rinse. Do this daily for at least 4–6 weeks.
Step 2: Audit and Simplify Your Skincare
Remove any products containing high concentrations of fatty acids that feed Malassezia. Keep your routine minimal and fungal-acne-safe. A basic routine works better than a complex one when you’re fighting fungal acne.
Step 3: Address Your Lifestyle Triggers
- Shower immediately after workouts — don’t let sweat sit on your skin
- Wash your pillowcase 2–3 times per week
- Avoid wearing hats or helmets for long periods without cleansing after
- Keep your hair clean and off your forehead
- Choose oil-free, non-comedogenic sunscreen
Step 4: See a Dermatologist If It Persists
Over-the-counter antifungals work for mild to moderate cases. If your fungal acne doesn’t improve after 6 weeks of targeted treatment, a dermatologist can prescribe oral antifungals like fluconazole. Don’t suffer in silence — this condition is very treatable with the right medical support.
Expert Commentary: Board-certified dermatologists consistently emphasize that correctly diagnosing fungal acne before starting treatment is the single most important step — and this video breaks that process down clearly.

A simple, fungal-acne-safe skincare routine can make a dramatic difference within weeks.
Frequently Asked Questions
What does fungal acne on the forehead look like?
Fungal acne on the forehead typically appears as small, uniform, itchy bumps. They are usually the same size, clustered together, and don’t respond to regular acne treatments. The bumps are often flesh-colored or slightly red and may feel rough to the touch.
What causes fungal acne on the forehead?
Fungal acne is caused by an overgrowth of Malassezia yeast on the skin. Factors like sweating, humidity, wearing hats or helmets, using heavy moisturizers, and taking antibiotics can all trigger this overgrowth on the forehead.
How do I treat fungal acne on my forehead?
Treatment includes using antifungal cleansers with ketoconazole or selenium sulfide, avoiding fatty acids and oils that feed Malassezia, and adopting a simplified skincare routine. Severe cases may need a prescription from a dermatologist.
Is fungal acne contagious?
No. Fungal acne is not contagious. Malassezia yeast naturally lives on everyone’s skin. The problem occurs when it overgrows due to specific conditions like excess oil, heat, or a disrupted skin microbiome.
Can regular acne products make fungal acne worse?
Yes. Many regular acne products contain oils and fatty acids that feed Malassezia yeast. Using the wrong products can make fungal acne significantly worse. Always check ingredient labels if you suspect fungal acne is your issue.
My Top Recommended Gear
These are the three product types that I consistently recommend to anyone starting their fight against fungal acne on the forehead. Always patch-test before committing to anything new.

Antifungal Ketoconazole Cleanser
The foundation of any fungal acne treatment routine. Ketoconazole directly targets Malassezia yeast. Use it daily and let it sit on skin for 60–90 seconds before rinsing for best results.🛒 View on Amazon
Fungal Acne-Safe Gel Moisturizer
A lightweight, oil-free gel moisturizer that hydrates your skin without feeding Malassezia. Look for formulas free from fatty acids, fermented ingredients, and heavy oils.🛒 View on Amazon
Selenium Sulfide Shampoo (as Cleanser)
A classic, affordable, and highly effective antifungal option. Many dermatologists recommend using selenium sulfide shampoo as a body wash or forehead treatment for Malassezia folliculitis.🛒 View on Amazon
The bottom line? Fungal acne on the forehead is not a life sentence. It’s a fixable problem — once you correctly identify it. Use these 7 warning signs as your personal checklist. Trust the process. The right treatment for the right diagnosis works every single time.
If you still feel unsure about what type of skin condition you’re dealing with, revisit the basics by exploring all the main types of acne — clarity there makes every treatment decision easier.
Amazon Affiliate Disclaimer: This site is a participant in the Amazon Services LLC Associates Program, an affiliate advertising program designed to provide a means for sites to earn advertising fees by advertising and linking to Amazon.com. As an Amazon Associate, I earn from qualifying purchases. This means if you click on certain product links and make a purchase, I may receive a small commission at no additional cost to you. I only recommend products I believe can be genuinely helpful. Always consult a qualified dermatologist or healthcare professional before starting any new skincare treatment.