Adult Acne Solutions for Clearer, Healthier Skin
Let’s get something straight: adult acne is not a teenage problem that somehow followed you home. It’s a full-blown, legitimate skin condition that affects roughly 50 million Americans every year, with a significant chunk of those being adults well into their 30s, 40s, and beyond. If you’ve ever stared at a fresh jawline breakout the morning of an important meeting and thought “Seriously?!” — you’re in very good company.
Here’s the problem: most acne advice online was written for teenagers dealing with T-zone oil slicks, not for adults juggling hormonal shifts, stress cortisol spikes, and a skincare cabinet full of products that may actually be making things worse. The agitation? You’ve probably tried everything — the fancy serums, the harsh scrubs, maybe even the toothpaste trick your cousin swore by — and your skin still isn’t cooperating. The solution? Understanding exactly what’s driving your acne and building a targeted, evidence-based strategy around that. That’s precisely what I’m going to walk you through here.
Table of Contents
- What Is Adult Acne and Why Does It Keep Coming Back?
- The Real Causes of Adult Acne (It’s Not Just Dirty Skin)
- Breaking Down the Types: Blackheads, Whiteheads, Cysts, and More
- Building a Skincare Routine That Actually Works for Acne-Prone Skin
- The Most Effective Acne Treatments Available Today
- Myth-Busting: What Everyone Gets Wrong About Adult Acne
- Frequently Asked Questions About Adult Acne
- My Top Recommended Gear
What Is Adult Acne and Why Does It Keep Coming Back?
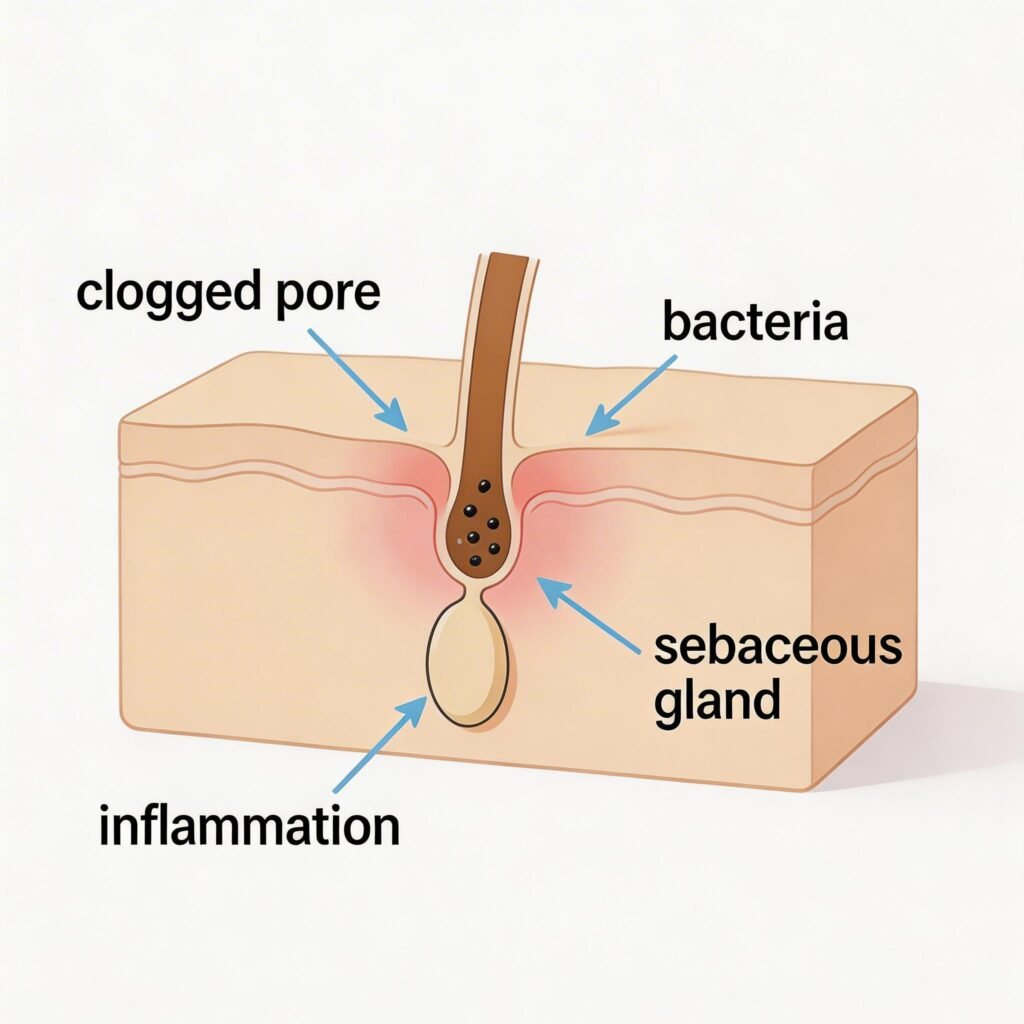
Quick Answer: Adult acne refers to acne that develops or persists after age 25. It occurs when hair follicles become clogged with sebum and dead skin cells, triggering inflammation and bacterial growth. Unlike teen acne, it’s often driven by hormones, stress, and lifestyle factors rather than puberty alone, making it both persistent and frustrating to treat without the right strategy.
Acne, at its core, is a disease of the hair follicle. When excess sebum (your skin’s natural oil) mixes with dead skin cells and plugs a pore, you’ve got a comedone. When bacteria — specifically Cutibacterium acnes — colonize that blocked follicle, your immune system fires up, and you get the red, inflamed breakouts that can linger for weeks. The reason adult acne is particularly stubborn is that the triggers are systemic, not just topical. You can wash your face twice a day religiously and still break out if your hormones, gut health, or stress levels are out of whack.
Understanding the specific pattern and type of your acne is the essential first step. I always recommend starting with a solid overview of the different acne types before you invest a single dollar in any treatment product. Guessing wrong is expensive and counterproductive.
The Real Causes of Adult Acne (It’s Not Just Dirty Skin)
I’ll say this once loudly for the people in the back: adult acne is not caused by poor hygiene. Over-washing actually strips your skin barrier and triggers rebound oil production that makes breakouts worse. So what actually causes it? Here’s what the evidence points to:
- Hormonal fluctuations: Androgens like testosterone stimulate sebaceous glands to produce more oil. This is why women often break out around their menstrual cycle, during pregnancy, or approaching menopause. I cover this in depth in the section on hormonal acne — it’s nuanced and worth understanding fully.
- Chronic stress: Cortisol, the stress hormone, directly increases sebum production and promotes inflammation. The NIH has published research confirming the stress-acne connection. Stress doesn’t just affect your mood; it literally shows up on your face.
- Diet: High-glycemic foods spike insulin, which raises androgen levels, which ramps up oil production. Dairy — particularly skim milk — has also been associated with acne flares in multiple studies.
- Comedogenic products: Your moisturizer, foundation, or hair product might be clogging your pores without you realizing it. IMO, this is one of the most underdiagnosed causes of persistent adult acne.
- Gut microbiome imbalance: Emerging research from institutions like the Harvard Health blog suggests that gut health influences skin inflammation through the gut-skin axis — a connection that’s increasingly hard to ignore.
- Medications: Corticosteroids, lithium, and some B vitamins (in high doses) can trigger or worsen acne as a side effect.
If you’re not sure where to start or what type of acne you’re dealing with, the start here guide is genuinely the smartest place to begin your journey. No filler, just a clear diagnostic framework.
Breaking Down the Types: Blackheads, Whiteheads, Cysts, and More
Not all acne plays by the same rules, which is exactly why one-size-fits-all treatments so often fail. Here’s a practical breakdown:
- Blackheads (open comedones): These are clogged pores where the top is open and the contents oxidize, turning dark. Contrary to popular belief, the black color isn’t dirt — it’s melanin reacting to oxygen.
- Whiteheads (closed comedones): Clogged pores where the opening is sealed over with skin. They appear as small, flesh-colored or white bumps. Both blackheads and whiteheads fall under comedonal acne, which responds well to retinoids and salicylic acid.
- Papules and pustules: These are inflammatory breakouts — red, tender bumps (papules) or red bumps with a white pus center (pustules). Benzoyl peroxide and topical antibiotics are typically effective here.
- Nodules and cysts: The heavy hitters. Deep, painful, often leaving scars if improperly treated. Cystic acne usually requires prescription-strength treatment, and squeezing it is one of the worst things you can do — I cannot stress this enough.
Knowing exactly what you’re dealing with lets you pick the right weapon from the arsenal. Treating cystic acne with a pore strip is like bringing a spoon to a swordfight. 😅
Building a Skincare Routine That Actually Works for Acne-Prone Skin
A solid skincare routine for acne-prone skin doesn’t need to be complicated — in fact, complexity is often the enemy. The more products you layer on, the harder it becomes to identify what’s helping and what’s hurting. Here’s the framework I recommend:
Morning Routine
- Gentle cleanser: Look for a non-stripping formula with a pH between 4.5 and 6. Avoid sulfates on sensitive or compromised skin.
- Vitamin C serum (optional but powerful): Antioxidant protection plus help fading post-acne hyperpigmentation. Apply before moisturizer.
- Oil-free, non-comedogenic moisturizer: Even oily, acne-prone skin needs hydration. Dehydrated skin overproduces oil in compensation — a vicious cycle.
- Broad-spectrum SPF 30+ sunscreen: Non-negotiable. Many acne treatments increase photosensitivity, and UV exposure darkens post-acne marks significantly.
Evening Routine
- Double cleanse (if you wear sunscreen or makeup): Oil-based cleanser first, then your gentle cleanser.
- Targeted treatment: This is where salicylic acid, benzoyl peroxide, or a retinoid comes in — but not all three at once. Start with one active at a time and introduce slowly.
- Moisturizer: Apply on slightly damp skin to lock in hydration, especially if you’re using a retinoid.
One insider tip I give everyone: change your pillowcase every 2–3 days. Your pillow accumulates oil, dead skin, and bacteria nightly and presses it back against your face for 7–8 hours. It’s one of those unsexy habits that actually moves the needle on clear skin tips.
The Most Effective Acne Treatments Available Today
Let’s talk about what’s actually in the evidence-based toolkit for acne treatment. I’ll break it down from OTC to prescription:
Over-the-Counter Actives
- Salicylic acid (BHA): Oil-soluble and exceptional at penetrating and exfoliating inside the pore. Ideal for blackheads and whiteheads. Concentrations between 0.5%–2% are effective for daily use.
- Benzoyl peroxide: Kills acne bacteria and reduces inflammation. Available in 2.5%–10% concentrations. The FDA notes that rare hypersensitivity reactions can occur, so patch-test before committing.
- Niacinamide: Reduces sebum production, minimizes pore appearance, calms redness, and plays beautifully with most other actives. My personal everyday workhorse.
- Adapalene (Differin): Now available OTC in the U.S. at 0.1%. It’s a retinoid that normalizes cell turnover and prevents pore clogging at the source. Consistent use over 12 weeks delivers significant results.
Prescription Options
- Tretinoin: The gold standard retinoid. Faster and more potent than adapalene, but requires a prescription and a break-in period.
- Spironolactone: An androgen blocker that works particularly well for hormonal jawline and chin acne in women. Many dermatologists consider it the most underutilized tool for adult female acne.
- Oral antibiotics: Effective short-term for inflammatory acne, but not a long-term solution given antibiotic resistance concerns.
- Isotretinoin (Accutane): Reserved for severe, treatment-resistant cases. Genuinely life-changing for those who qualify, with a strict monitoring protocol.
For a comprehensive overview of all options, the acne treatments guide covers both topical and systemic approaches in granular detail — worth a full read before your next derm appointment.
Expert Commentary: This dermatologist-led breakdown cuts through the noise on adult acne triggers and treatment priorities, giving you the clinical perspective you’d normally only get inside a paid consultation — worth every minute of your time.

Myth-Busting: What Everyone Gets Wrong About Adult Acne
Let’s destroy some deeply entrenched myths that I see derailing people’s progress constantly:
- Myth: Sunscreen causes acne. Reality: The wrong sunscreen can clog pores, but modern non-comedogenic mineral or lightweight chemical sunscreens are safe and essential. Skipping SPF makes acne scars and hyperpigmentation dramatically worse.
- Myth: You need to “dry out” your skin to treat acne. Reality: Dehydration is one of the fastest ways to worsen acne. Stripped skin produces more oil to compensate, and a compromised barrier can’t defend against bacteria.
- Myth: Natural and DIY remedies are safer. Reality: Lemon juice, apple cider vinegar, and baking soda are all the wrong pH for your skin and can cause chemical burns or severe irritation. “Natural” does not automatically mean safe or effective.
- Myth: Adult acne always goes away on its own. Reality: Without addressing the underlying trigger — whether hormonal, dietary, or product-related — adult acne can persist indefinitely and cause lasting scarring. Proactive treatment beats the “wait and see” approach every time.
- Myth: Popping pimples speeds up healing. Reality: Squeezing pushes bacteria and debris deeper into surrounding tissue, extends healing time by days, and significantly increases the risk of permanent scarring. Hard pass.
The National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS) provides excellent evidence-based resources if you want to fact-check any of these against primary scientific sources. And honestly, you should — skepticism is a healthy skincare habit.
Here’s the question I want you to sit with: How much money have you spent on products that targeted the symptoms of your acne rather than the root cause? If the number makes you wince, you’re not alone — and that’s exactly why the education piece matters as much as the product selection.
Frequently Asked Questions About Adult Acne
Why do adults get acne?
Adults get acne due to a combination of hormonal fluctuations, stress, diet, clogged pores, and sometimes comedogenic skincare or makeup products. Unlike teenage acne, adult acne often concentrates along the jawline and chin and tends to be more inflammatory in nature.
What is the best acne treatment for adults?
The best acne treatment for adults depends on the acne type. Topical retinoids, salicylic acid, benzoyl peroxide, and niacinamide work well for most. Hormonal acne may require prescription options like spironolactone or oral contraceptives. Always consult a dermatologist for persistent or severe cases.
Can diet cause adult acne?
Yes. High-glycemic foods, dairy, and diets loaded with processed sugars can spike insulin and androgen levels, which in turn stimulates excess sebum production. Research published by the American Academy of Dermatology supports the link between diet and acne flares.
How long does it take for adult acne to clear up?
With a consistent and correctly chosen skincare routine, most adults see noticeable improvement within 6–12 weeks. Severe cases, particularly cystic or hormonal acne, may take 3–6 months of targeted treatment under medical supervision.
Are blackheads and whiteheads different from other types of acne?
Yes. Blackheads (open comedones) and whiteheads (closed comedones) are non-inflammatory acne caused by clogged pores filled with dead skin cells and sebum. They differ from inflammatory acne like papules, pustules, or cysts, which involve bacteria and immune response. TBH, getting this distinction right is half the battle in choosing the right treatment approach.
My Top Recommended Gear
These are the product categories that consistently deliver results for adult acne. I link to Amazon searches so you can compare top-rated options yourself and read real reviews:
- Salicylic Acid Face Cleanser: A non-negotiable foundation for any acne-prone skincare routine. Keeps pores clear daily without stripping your barrier.
→ Browse Salicylic Acid Cleansers on Amazon - Benzoyl Peroxide Spot Treatment: Targeted, fast-acting bacteria-killer for active inflammatory breakouts. Choose 2.5% to minimize irritation without sacrificing efficacy.
→ Browse Benzoyl Peroxide Spot Treatments on Amazon - Non-Comedogenic Moisturizer with Niacinamide: Hydrates without clogging pores and actively works to reduce sebum production and redness — a rare and powerful combination.
→ Browse Non-Comedogenic Niacinamide Moisturizers on Amazon
Disclaimer: This post contains affiliate links. As an Amazon Associate, I may earn a commission from qualifying purchases at no additional cost to you. All product recommendations are based on research and expertise, not compensation from brands. This article is for informational purposes only and does not constitute medical advice. Consult a licensed dermatologist for personalized treatment guidance.







