Cystic Acne: 10 Powerful Ways to Calm Fast
Let’s be real, cystic acne isn’t just a breakout. It’s a deep, painful, ego-bruising invasion that sits beneath your skin like it pays rent. If you’ve ever woken up to a jawline that looks like a topographic map, you know exactly what I mean. The problem is that most advice online is either laughably basic (“drink more water!”) or dangerously wrong. So let’s fix that. Right now.
Here’s what makes cystic acne particularly nasty: it doesn’t respond to the surface-level spot treatments that handle regular pimples. These lesions form deep in the dermis, meaning your standard salicylic acid face wash barely touches them. The result? Weeks of inflammation, a real risk of permanent scarring, and a growing sense that your skin is just… broken. It isn’t — but you do need a smarter approach.
I’ve spent over a decade studying acne skincare, interviewing dermatologists, and testing products that promise the world. In this guide, I give you 10 evidence-backed, no-nonsense strategies to calm cystic acne fast — and actually keep it gone.
Table of Contents
- What Exactly Is Cystic Acne?
- The Root Causes You Need to Know
- Way #1 — Ice Therapy: The Free, Instant Fix
- Way #2 — Benzoyl Peroxide Done Right
- Way #3 — Retinoids: The Long Game That Wins
- Way #4 — Target the Hormonal Root Cause
- Way #5 — The Cortisone Injection Shortcut
- Way #6 — Audit Your Diet Ruthlessly
- Way #7 — Salicylic Acid as a Daily Preventive
- Way #8 — Manage Stress Before It Manages Your Skin
- Way #9 — Rebuild Your Skin Barrier
- Way #10 — When to Consider Isotretinoin
- FAQ: Your Burning Questions Answered
- My Top Recommended Gear
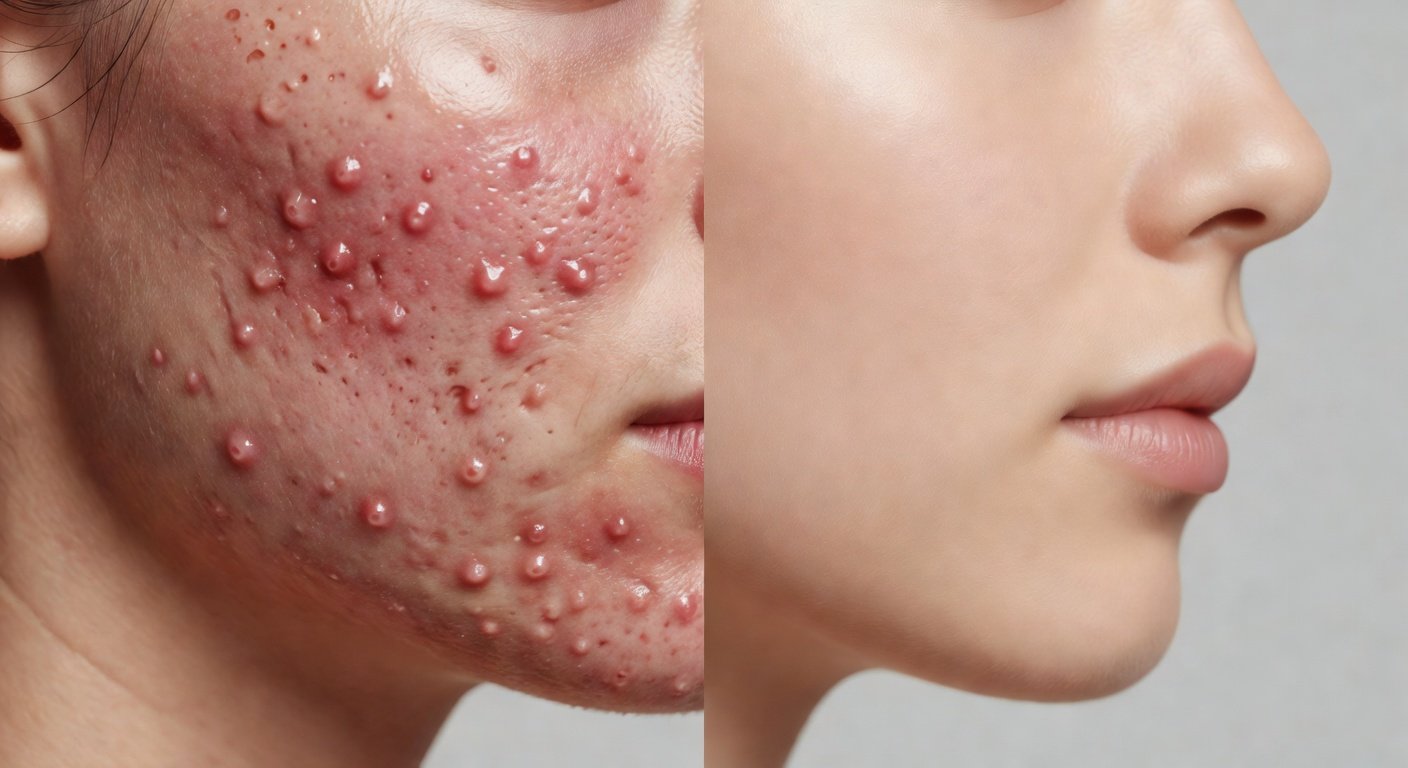
What Exactly Is Cystic Acne?
Quick Answer: Cystic acne is the most severe form of acne vulgaris. It forms when a pore becomes deeply blocked with oil, dead skin cells, and bacteria, triggering a significant immune response beneath the skin’s surface. The result is a large, painful, fluid-filled cyst that cannot be popped safely and often causes scarring if mishandled.
Think of cystic acne as the “final boss” of the acne world. According to the American Academy of Dermatology, cystic lesions are classified as severe inflammatory acne — the kind that requires more than a drugstore fix. Unlike whiteheads or blackheads, cysts develop several layers below the skin surface, which is precisely why they hurt when you touch them and why squeezing does more harm than good.
Want to understand all the variations in play? This breakdown of acne types will give you a clearer picture of where cystic acne sits in the spectrum and why it demands a different treatment protocol entirely.
The Root Causes You Need to Know
Before you can fix something, you need to understand why it’s broken. Cystic acne causes aren’t random — they follow predictable patterns that, once you identify them, become much easier to address.
- Hormonal surges: Androgens like testosterone stimulate sebaceous glands to produce excess oil. This is the #1 driver of cystic breakouts in adults, especially women during their menstrual cycle.
- Genetics: If your parents had cystic acne, your follicle structure may be more prone to deep blockages. Sorry — but knowing this helps you plan ahead.
- High-glycemic diet: Research published by the National Institutes of Health links high-glycemic foods to increased IGF-1 levels, which directly stimulate oil production.
- Stress hormones: Cortisol is a sneaky villain. It upregulates oil gland activity and triggers inflammatory cascades — a double punch for acne-prone skin.
- Wrong skincare products: Using comedogenic moisturizers or heavy silicone-based primers is basically feeding the beast.
Not sure where to start with your own skin assessment? The Start Here guide walks you through identifying your specific triggers in a structured, logical way — no guesswork needed.
Way #1 — Ice Therapy: The Free, Instant Fix
I know ice doesn’t sound glamorous, but hear me out. Applying cold directly to a cystic lesion causes vasoconstriction — meaning the blood vessels beneath constrict, which immediately reduces swelling and dulls pain. Wrap an ice cube in a clean cloth (never apply bare ice to skin) and hold it over the cyst for 10-minute intervals, three times daily.
This won’t cure the cyst, but it buys you critical time by reducing the inflammatory response before it snowballs. Think of it as damage control on day one. Zero cost, zero side effects. IMO, this is the most underrated step in the entire cystic acne toolkit.
Way #2 — Benzoyl Peroxide Done Right
Benzoyl peroxide (BP) is one of the most clinically validated acne treatment ingredients on the planet. It works by releasing oxygen into the pore, creating a hostile environment for Cutibacterium acnes (the bacteria that drives inflammation). The critical mistake most people make? Using too high a concentration and applying it across the entire face.
For cystic acne, I recommend a 2.5% to 5% concentration applied as a targeted spot treatment — not a full-face wash. Higher concentrations (10%) don’t work better; they just cause more irritation and compromise your skin barrier. A compromised barrier means more inflammation. See the problem?
Way #3 — Retinoids: The Long Game That Wins
If cystic acne has been a recurring problem for you — not just occasional — you need a retinoid in your routine. Retinoids (vitamin A derivatives like tretinoin or adapalene) accelerate cellular turnover, which prevents the dead skin cell buildup that clogs pores in the first place. They also regulate sebum production over time.
Adapalene 0.1% is now available over the counter in the US and is one of the best-studied topical retinoids for acne, per the FDA. Start with every-other-night application to avoid the dreaded “retinoid purge” — a temporary worsening that makes beginners quit too early. Stick with it for 12 weeks before judging results.
Explore the full landscape of options — from OTC to prescription — in this detailed acne treatments resource I recommend as required reading before you invest in any new product.
Way #4 — Target the Hormonal Root Cause
Are your breakouts consistently worse the week before your period? Do they cluster on your chin and jawline? That’s your body waving a hormonal flag. Topical treatments alone won’t cut it — you need to address the upstream problem.
Spearmint tea, taken twice daily, has shown in small studies to reduce androgen levels in women with PCOS-related acne. Zinc supplementation (30mg elemental zinc daily) also demonstrates meaningful anti-androgen and anti-inflammatory effects. For more aggressive cases, a dermatologist or OB-GYN can prescribe spironolactone — an oral androgen blocker with an impressive track record for hormonal cystic acne in adult women.
I’ve written extensively about this on the site’s dedicated hormonal acne page — it’s worth a thorough read if this section resonated with you 🙂
Way #5 — The Cortisone Injection Shortcut
This is the nuclear option — in the best way possible. A dermatologist-administered intralesional cortisone injection (triamcinolone acetonide, diluted appropriately) can flatten even an angry, volcano-sized cyst within 24 to 48 hours. This isn’t a myth or an exaggeration; it’s a well-established procedure that I consider the single fastest legitimate solution for a severe, isolated cystic lesion.
The risks? If administered at too high a concentration, you can get temporary skin atrophy (a small indentation). That’s why you want a board-certified dermatologist doing this — not someone doing it “on the cheap.” One visit, roughly $50–$150 out of pocket at most clinics, and that monster is gone before your next social engagement. Worth every penny if you have a big event coming up.
Way #6 — Audit Your Diet Ruthlessly
I’ll be direct: the “diet doesn’t affect acne” myth is dead. Multiple peer-reviewed studies now link high-glycemic foods, dairy (especially skim milk), whey protein supplements, and excess iodine to acne flares. The mechanism involves insulin-like growth factor 1 (IGF-1), which ramps up sebum production and skin cell proliferation simultaneously.
My personal approach? I ran a two-week elimination of dairy and high-GI foods (white bread, sugary drinks, processed snacks) while tracking breakout frequency. The difference was measurable. This isn’t about being precious with your food — it’s about collecting data on your own biology. Eat whole foods, prioritize low-GI carbohydrates like sweet potatoes and legumes, and keep a simple food-skin journal for 30 days.
Expert Commentary: This dermatologist-led breakdown cuts through the noise with clinical precision — watch it specifically for the segment on why over-the-counter treatments fail for deep cystic lesions and what to ask your dermatologist for instead.
Way #7 — Salicylic Acid as a Daily Preventive
Salicylic acid (BHA) is lipid-soluble, meaning it penetrates into the pore lining and dissolves the sebum and cellular debris that cause blockages. At 0.5% to 2%, used as a daily cleanser or toner, it’s one of the most effective preventive tools for acne-prone skin. Note the word preventive — salicylic acid won’t dramatically shrink an existing deep cyst, but it stops new ones from forming by keeping pores clear.
Pair it with your retinoid strategically: BHA in the morning, retinoid at night. Don’t layer them in the same step — that’s a recipe for irritation and a damaged skin barrier. Clean the pipes daily, strengthen the walls at night. Simple, systematic, effective.
Way #8 — Manage Stress Before It Manages Your Skin
Have you ever noticed your skin explodes during exam season, a brutal work crunch, or after a rough relationship stretch? That’s not coincidence — cortisol directly stimulates neuropeptides that trigger sebaceous gland activity and systemic inflammation. Chronic stress keeps your cortisol elevated, which means your skin stays in a constant low-grade inflammatory state.
I’m not going to tell you to “just meditate” because that’s the kind of advice that makes people roll their eyes. What I will say is this: sleep 7–9 hours per night (non-negotiable for skin repair), incorporate 20 minutes of moderate cardio daily (proven to lower cortisol), and consider adaptogenic supplements like ashwagandha — which a 2012 study in the Indian Journal of Psychological Medicine found significantly reduced serum cortisol in chronically stressed adults.

Way #9 — Rebuild Your Skin Barrier
Here’s a myth I want to bust loudly: oily, acne-prone skin does not need to be stripped dry. Over-cleansing and using harsh, alcohol-heavy toners destroys the skin’s acid mantle — the protective lipid layer that keeps bacteria out and moisture in. When the barrier breaks down, skin paradoxically produces more oil to compensate, and the inflammatory response to bacteria intensifies.
The fix is counterintuitive but evidence-based: use a gentle, non-comedogenic moisturizer twice daily. Look for ceramides, niacinamide, and hyaluronic acid as active ingredients. Niacinamide in particular (5% concentration) regulates sebum production, reduces hyperpigmentation from old cysts, and has anti-inflammatory properties — making it one of the most versatile actives for stubborn acne skin types. Check out my product reviews for specific recommendations I’ve personally vetted.
Way #10 — When to Consider Isotretinoin
When everything else has failed — when you’ve done retinoids, antibiotics, hormonal therapy, diet overhauls, and still cycle through painful cysts every month — isotretinoin (formerly branded as Accutane) is the conversation to have with your dermatologist. This oral vitamin A derivative attacks cystic acne on every front simultaneously: it shrinks oil glands, normalizes skin cell shedding, eliminates acne bacteria, and reduces inflammation.
Yes, it has a significant side effect profile that demands medical supervision (mandatory blood tests, pregnancy prevention protocols, and monitoring for mood changes). But for severe, scarring cystic acne that hasn’t responded to anything else, the data from decades of clinical use shows remission rates of 85–90% after a full course. That’s not a treatment — that’s a cure for most people who use it appropriately.
The decision to pursue isotretinoin shouldn’t be taken lightly, but it also shouldn’t be feared into irrelevance by internet horror stories. Talk to a board-certified dermatologist with experience prescribing it. Ask the right questions. Weigh the real risk-benefit math for your specific situation.
FAQ: Your Burning Questions Answered
What causes cystic acne?
Cystic acne forms when excess sebum, dead skin cells, and bacteria become trapped deep within a pore, triggering a significant immune response. Hormonal fluctuations — particularly androgens — are a primary driver, which is why cystic breakouts so often cluster around the jawline and chin.
How long does cystic acne take to heal?
An individual cystic pimple can linger anywhere from 1 to 4 weeks without treatment. With the right targeted approach — ice therapy, topical retinoids, or a cortisone injection from a dermatologist — you can dramatically reduce inflammation within 24 to 72 hours.
Is cystic acne hormonal?
Very often, yes. Hormonal shifts caused by menstrual cycles, polycystic ovary syndrome (PCOS), stress, or puberty can spike androgen levels, which stimulate oil glands into overdrive. This makes hormonal cystic acne one of the most common — and most frustrating — presentations dermatologists treat.
Can I pop a cystic pimple?
No — and I can’t stress this enough. Cystic acne sits too deep beneath the skin surface to pop safely. Attempting to force it will rupture the follicle wall internally, spread infection to surrounding tissue, and nearly guarantee post-inflammatory hyperpigmentation and scarring. Hands off.
What is the fastest way to get rid of a cystic pimple?
The fastest proven method is a cortisone injection administered by a dermatologist, which can flatten a cyst within 24 hours. At home, wrapping ice in a cloth and applying it for 10-minute intervals reduces swelling immediately. Combining that with a benzoyl peroxide spot treatment accelerates the process significantly.
My Top Recommended Gear
These are the products I actually recommend to people dealing with stubborn, deep pimples. I’ve cross-referenced clinical data, ingredient lists, and real-world user feedback before putting any of these on this list.
- Adapalene 0.1% Retinoid Acne Gel — The gold-standard OTC retinoid for preventing cystic formations and normalizing cell turnover. Start slow, stay consistent.
- 2.5% Benzoyl Peroxide Spot Treatment — Clinically effective at killing acne bacteria without the unnecessary aggression of higher-strength formulas. My go-to for targeted application.
- Niacinamide + Ceramide Moisturizer for Acne-Prone Skin — Because every serious acne routine needs a barrier-repairing, sebum-regulating moisturizer that won’t clog a single pore. Non-negotiable. TBH, this category alone transforms most people’s routines.
Disclaimer: This post contains affiliate links. As an Amazon Associate, I may earn a commission from qualifying purchases at no additional cost to you. All product recommendations are based on independent research and personal experience. This content is for informational purposes only and does not constitute medical advice. Always consult a board-certified dermatologist for personalized medical treatment.