Hormonal Acne Hacks for Clearer, Calmer Skin
Let me guess: you’ve dealt with hormonal acne long enough to know it’s not your average teenage breakout. You wake up with a painful cyst on your chin right before an important meeting, and your jawline looks like a topographic map of inflammation. You’ve tried every acne remedy your Instagram feed has pitched, yet those hormonal breakouts keep showing up like clockwork.
Here’s the problem: most people treat hormonal acne like regular acne, slapping on benzoyl peroxide and hoping for the best. That approach fails because hormonal acne operates by completely different rules. The agitation? Every month you waste on the wrong acne treatment damages your skin barrier, deepens hyperpigmentation, and tanks your confidence.
The solution? I’m going to show you exactly how to tackle adult acne at its hormonal roots using strategies I’ve refined over a decade of research and real-world testing. No fluff, no miracle cures—just proven skincare tips that actually address what’s happening beneath your skin.
Table of Contents
- What Is Hormonal Acne (And Why Your Skin Hates You Right Now)
- The Root Causes: It’s Not Just “Bad Skin”
- How to Actually Identify Hormonal Acne
- Evidence-Based Treatment Strategies That Work
- Topical Solutions Worth Your Money
- Lifestyle Hacks That Move the Needle
- What NOT to Do (Myth-Busting Time)
- Frequently Asked Questions
- My Top Recommended Gear
What Is Hormonal Acne (And Why Your Skin Hates You Right Now)
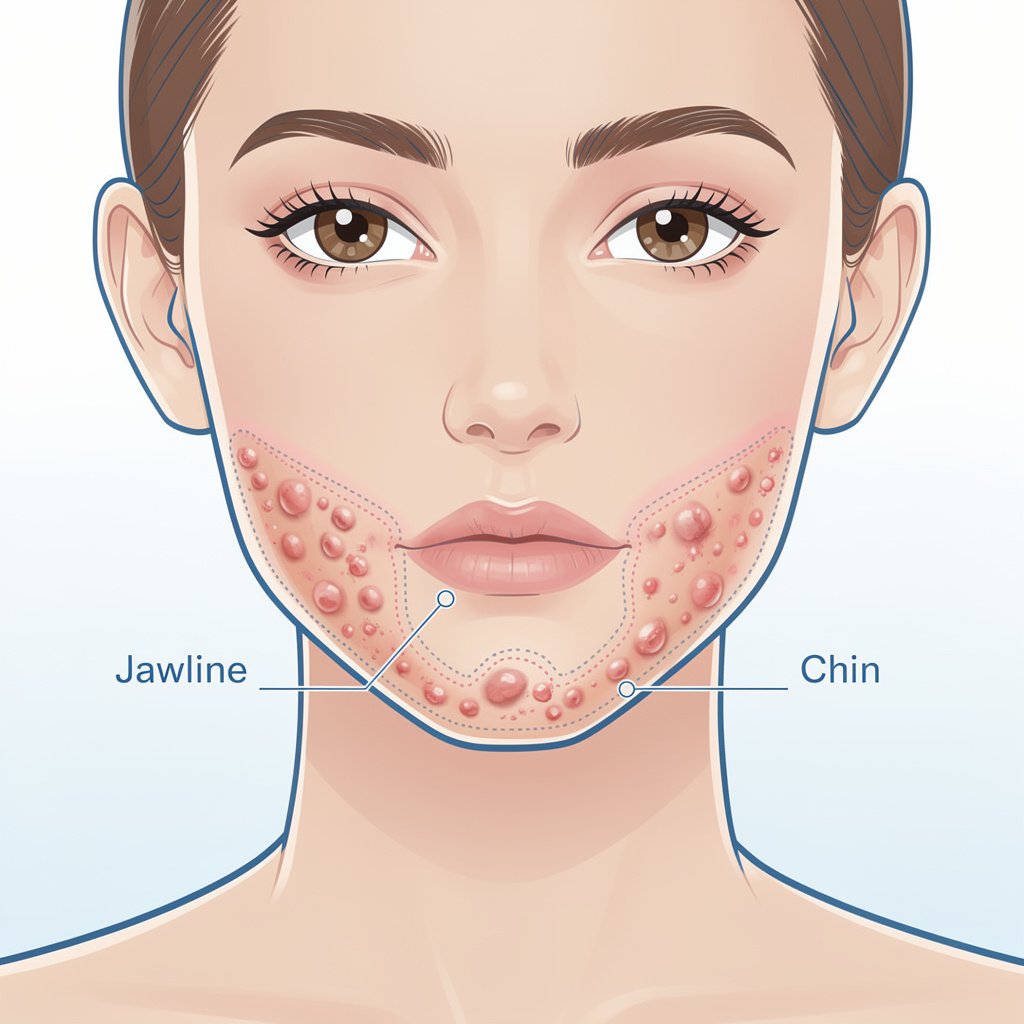
Hormonal acne is acne that develops or worsens in response to hormonal fluctuations in your body. Unlike the acne you might have experienced as a teenager, this variant shows up primarily along your lower face—the jawline, chin, and sometimes neck—following a predictable pattern tied to your menstrual cycle, stress levels, or life stages like perimenopause.
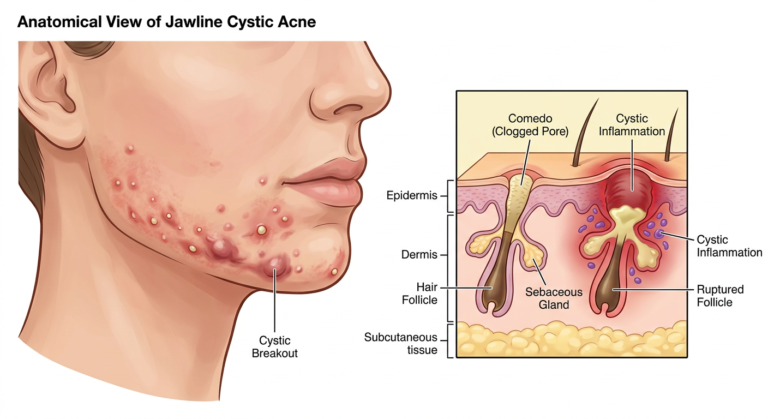
Your sebaceous glands contain androgen receptors that respond to hormones like testosterone. When these hormones surge (or when estrogen drops, creating a relative androgen excess), your glands pump out extra sebum. Mix that with dead skin cells, inflammation, and C. acnes bacteria, and you’ve got the perfect storm for those deep, painful cystic lesions that define hormonal breakouts.
Understanding the different types of acne helps you recognize that hormonal acne requires a fundamentally different approach than comedonal or bacterial acne.
The Root Causes: It’s Not Just “Bad Skin”
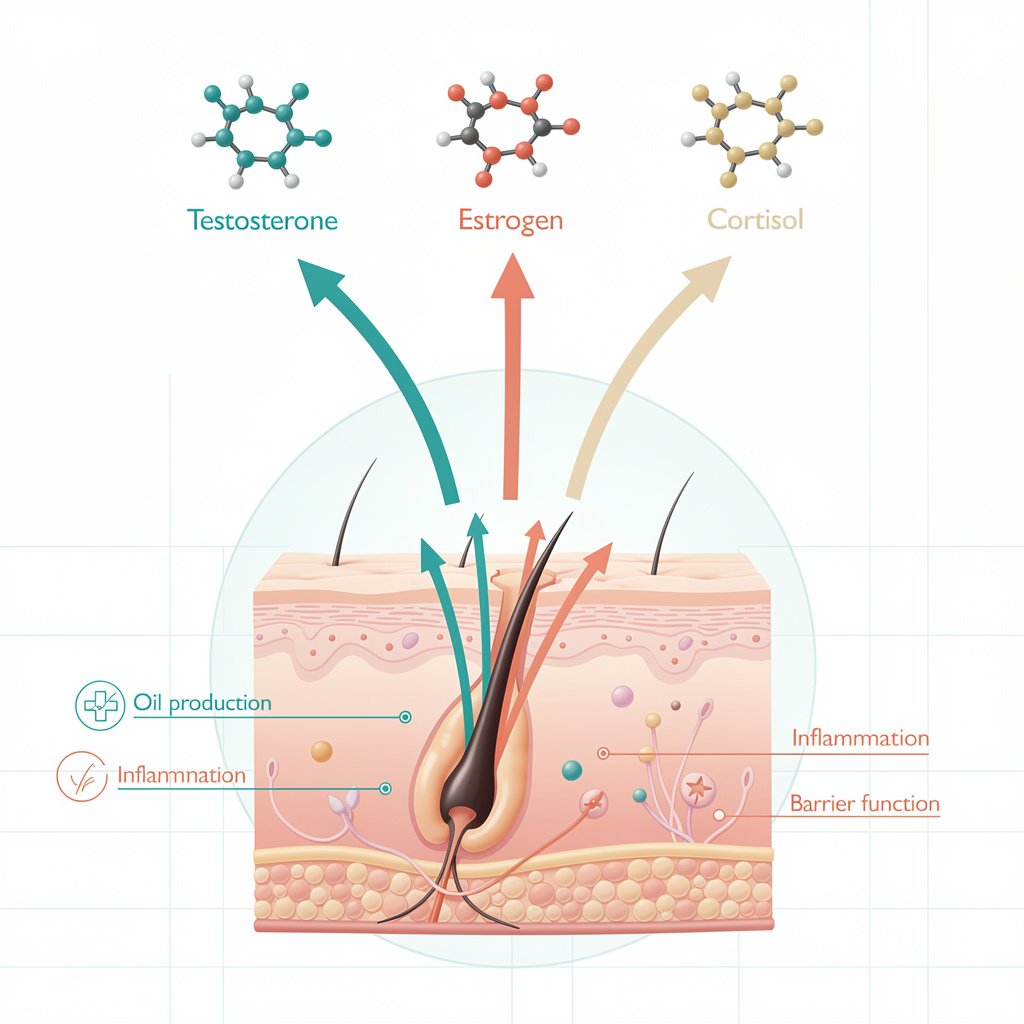
Several internal triggers drive hormonal acne, and recognizing yours matters more than any product you’ll buy:
- Menstrual Cycle Fluctuations: Progesterone rises during the luteal phase (days 14-28), stimulating sebum production. Meanwhile, estrogen drops, removing its protective anti-inflammatory effects.
- Polycystic Ovary Syndrome (PCOS): This endocrine disorder affects up to 10% of women and creates elevated androgens, insulin resistance, and persistent acne. According to the National Institutes of Health, PCOS is one of the leading causes of hormonal acne in adult women.
- Perimenopause and Menopause: Estrogen declines while testosterone remains relatively stable, creating that androgen dominance I mentioned earlier.
- Stress and Cortisol: Chronic stress elevates cortisol, which triggers inflammatory pathways and stimulates oil production. Your 3 AM anxiety sessions are literally breaking out your face.
- Dietary Factors: High-glycemic foods and dairy can spike insulin and IGF-1, both of which increase androgen activity. The American Academy of Dermatology acknowledges these dietary connections.
IMO, most people focus too much on external acne causes and ignore the internal biochemistry driving their breakouts. That’s why I always recommend starting with proper diagnosis—sometimes you need bloodwork to identify underlying hormonal imbalances.
How to Actually Identify Hormonal Acne
Not every pimple on your chin is hormonal. Here’s how you distinguish hormonal acne from other forms:
- Location, Location, Location: Hormonal acne clusters around the lower third of your face—jawline, chin, and sometimes upper neck. If your forehead looks like a minefield but your jaw is clear, that’s probably not hormonal.
- Timing: Does your skin go haywire 7-10 days before your period? That cyclical pattern is a dead giveaway.
- Lesion Type: Hormonal acne typically presents as deep, painful cysts rather than whiteheads or blackheads. These suckers hurt before you can even see them.
- Age of Onset: Starting or worsening after age 25? Probably hormonal, especially if you never had severe acne as a teenager.
- Treatment Resistance: If traditional acne treatments barely make a dent, hormones are likely the culprit.
If you’re still not sure where to start, check out this comprehensive starting guide that walks you through proper acne assessment.
Evidence-Based Treatment Strategies That Work
Here’s where I separate the wheat from the chaff. Effective hormonal acne treatment requires a multi-pronged approach addressing both internal hormones and external skin health.
Systemic Treatments (The Heavy Hitters)
Oral Contraceptives: Birth control pills containing both estrogen and progestin can regulate hormone fluctuations and reduce androgen activity. The FDA has approved several formulations specifically for acne treatment. You’ll typically see improvement after 3-4 months, though individual responses vary.
Spironolactone: This androgen blocker is my go-to recommendation for women with persistent hormonal acne. It works by blocking androgen receptors in your sebaceous glands, reducing oil production at the source. Most dermatologists start at 50-100mg daily. According to research published in the Journal of the American Academy of Dermatology, spironolactone shows significant improvement in about 80% of patients.
Isotretinoin (Accutane): For severe, scarring hormonal acne that doesn’t respond to other treatments, isotretinoin remains the gold standard. It permanently shrinks sebaceous glands and resets your skin’s oil production. Yes, the side effects are real, but for many people, it’s life-changing.
You’ll want to explore the full range of available acne treatments with a qualified dermatologist before committing to any systemic medication.
Topical Solutions Worth Your Money

While topicals alone won’t cure hormonal acne, they play a crucial supporting role in managing breakouts and preventing scarring:
Retinoids (Adapalene, Tretinoin): These vitamin A derivatives normalize skin cell turnover, prevent comedones, and reduce inflammation. I’ve written extensively about adapalene’s effectiveness for acne—it’s available over-the-counter at 0.1% and works remarkably well when combined with hormonal treatments. Start slow (every other night) and build tolerance.
Niacinamide: This B3 vitamin reduces inflammation, regulates sebum production, and improves skin barrier function. I recommend 5-10% concentrations applied morning and evening. It plays well with other actives and rarely causes irritation.
Azelaic Acid: This multitasker targets acne bacteria, reduces inflammation, and fades hyperpigmentation. It’s especially valuable for hormonal acne because it addresses both active breakouts and the dark marks they leave behind.
Benzoyl Peroxide (Strategic Use): While not a primary hormonal acne treatment, BP can help manage bacterial overgrowth during breakouts. I suggest short-contact therapy (apply for 5 minutes, then rinse) to minimize irritation.
Want to know which specific formulations actually work? Check out my detailed product reviews where I test and rate everything.
Lifestyle Hacks That Move the Needle
These aren’t sexy, but they’re effective. Lifestyle modifications can significantly impact hormonal balance and skin health:
Dietary Adjustments
Reduce high-glycemic foods (white bread, sugary snacks, processed carbs) that spike insulin. Consider eliminating dairy for 4-6 weeks to assess your response—many people see dramatic improvement. Increase omega-3 fatty acids from fish, walnuts, or supplements to combat inflammation.
Stress Management
Chronic stress wreaks absolute havoc on hormones. I know “just relax” sounds useless, but implementing actual stress-reduction practices—meditation, regular exercise, adequate sleep, therapy—produces measurable cortisol reduction. Your skin will thank you.
Sleep Hygiene
Poor sleep disrupts cortisol rhythms, increases inflammation, and impairs skin repair. Aim for 7-9 hours nightly. Change your pillowcase every 2-3 days to reduce bacterial transfer.
Exercise (The Right Kind)
Moderate exercise improves insulin sensitivity and reduces stress hormones. However, excessive high-intensity training can actually increase cortisol and worsen hormonal acne. Balance is key.
This dermatologist breaks down the hormonal mechanisms behind adult acne and explains why standard treatments often fail—worth watching for the section on androgen receptors alone.
What NOT to Do (Myth-Busting Time)
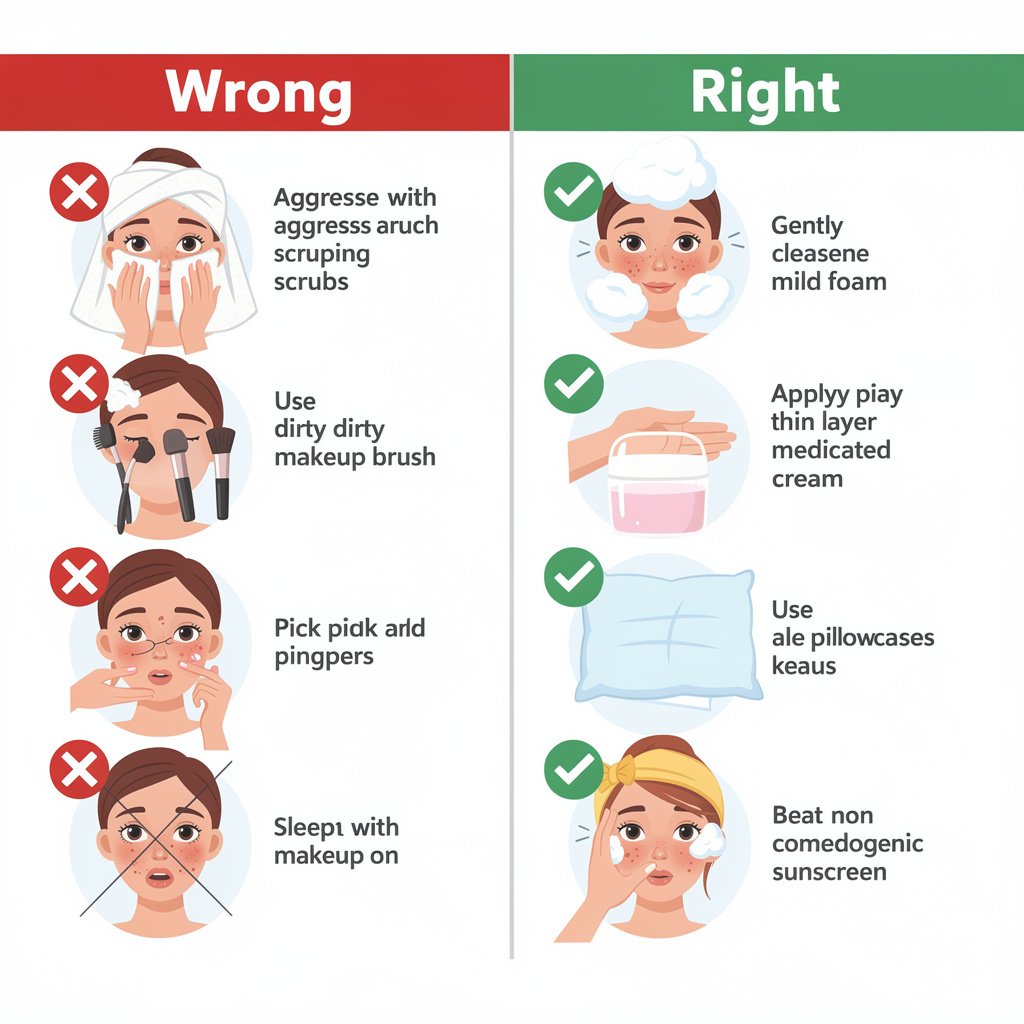
Let’s kill some common misconceptions that keep people stuck in the hormonal acne cycle:
Myth: You can “detox” hormonal acne with charcoal masks and fancy scrubs.
Reality: Hormonal acne originates from internal hormone fluctuations. No amount of external “detoxing” will fix internal biochemistry. You’re just irritating your skin barrier for Instagram aesthetics.
Myth: Hormonal acne only affects women.
Reality: Men absolutely get hormonal acne, especially related to testosterone fluctuations, steroid use, or stress-induced cortisol spikes. The presentation may differ, but the underlying mechanisms are similar.
Myth: You should dry out hormonal acne with harsh products.
Reality: Stripping your skin triggers compensatory oil production and damages your moisture barrier. This creates more inflammation and makes your skin more vulnerable to breakouts. Use gentle, barrier-supporting products instead.
Myth: Diet doesn’t matter.
Reality: While diet alone won’t cure hormonal acne, it significantly influences insulin, IGF-1, and inflammatory pathways. Pretending food choices don’t affect skin is scientifically inaccurate.
Myth: Natural remedies work as well as prescription treatments.
Reality: Look, I appreciate a good tea tree oil as much as anyone, but for moderate-to-severe hormonal acne, you need prescription-strength interventions. Tea tree won’t block androgen receptors or normalize sebaceous gland activity. Use natural remedies as complementary tools, not primary treatments.
Frequently Asked Questions
What causes hormonal acne in adults?
Hormonal acne develops when fluctuations in androgens, estrogen, and progesterone trigger excess sebum production. This happens during menstrual cycles, pregnancy, perimenopause, or due to conditions like PCOS. Stress-induced cortisol spikes and insulin resistance from dietary factors also contribute to hormonal imbalances that manifest as acne.
How is hormonal acne different from regular acne?
Hormonal acne typically appears along the jawline, chin, and lower cheeks in a characteristic pattern. It flares cyclically with hormonal changes and often presents as deep, painful cystic lesions rather than surface-level breakouts. Regular acne may appear anywhere on the face and doesn’t necessarily follow a predictable cycle.
What is the most effective treatment for hormonal acne?
The most effective treatments combine topical retinoids like adapalene with hormonal therapies such as spironolactone or birth control pills. A comprehensive approach addressing both internal hormones and external skincare yields the best results. For severe cases, isotretinoin may be necessary.
Can men get hormonal acne?
Absolutely. Men experience hormonal acne related to testosterone fluctuations, stress-induced cortisol elevation, or anabolic steroid use. While the hormonal mechanisms differ slightly from women, the treatment principles remain similar—address the internal hormone imbalance while supporting skin health externally.
How long does it take to see results from hormonal acne treatment?
Most hormonal acne treatments require 3-6 months to show significant improvement. Oral contraceptives typically take 3-4 months, spironolactone may show results in 6-8 weeks but continues improving for months, and retinoids need at least 12 weeks. Patience is essential—your skin didn’t break out overnight, and it won’t clear overnight either.
Should I avoid certain foods if I have hormonal acne?
Research suggests limiting high-glycemic foods, dairy products, and excessive sugar intake may help reduce hormonal acne severity. These foods influence insulin and IGF-1 levels, which affect androgen activity. Try eliminating dairy for 4-6 weeks and reducing refined carbohydrates to assess your individual response.
My Top Recommended Gear
After testing countless products, here are my top recommendations for managing hormonal acne:
- Differin Adapalene Gel 0.1% – The only FDA-approved over-the-counter retinoid for acne. Start here before moving to prescription-strength options.
- La Roche-Posay Toleriane Hydrating Gentle Cleanser – Gentle enough for sensitized hormonal acne skin while effectively removing impurities without stripping your barrier.
- CeraVe Moisturizing Cream – Non-comedogenic, ceramide-rich formula that supports skin barrier function during aggressive acne treatment. Essential for preventing that tight, irritated feeling.
Disclaimer: This post contains affiliate links. As an Amazon Associate, I may earn a commission from qualifying purchases at no additional cost to you.