When to See a Dermatologist for Acne: 7 Clear Signs
Figuring out when to see a dermatologist for acne is something most people overthink—and I get it. You’ve spent months (maybe years) cycling through drugstore cleansers, trendy serums, and TikTok “miracle hacks” that promised clear skin but delivered disappointment. Your bathroom shelf looks like a skincare graveyard, your skin is angry, and you’re wondering if you’re just doing something wrong. Here’s the truth I wish someone had told me years ago: sometimes the smartest skincare move isn’t another product—it’s picking up the phone and booking a dermatology appointment. The seven signs below will tell you exactly when that moment has arrived.
Table of Contents
- When Should You Actually See a Dermatologist for Acne?
- Sign #1: Over-the-Counter Products Have Stopped Working
- Sign #2: You’re Dealing with Cystic Acne
- Sign #3: Acne Scarring Is Getting Worse
- Sign #4: Your Acne Is Wrecking Your Mental Health
- Sign #5: You’re an Adult and Acne Won’t Quit
- Sign #6: You Suspect a Hormonal Imbalance
- Sign #7: You’ve Developed Sudden, Severe Acne
- What to Expect at Your First Dermatology Appointment
- Frequently Asked Questions
- My Top Recommended Gear
When Should You Actually See a Dermatologist for Acne?
You should see a dermatologist for acne when over-the-counter treatments fail after 8–12 consistent weeks, when you develop painful cystic breakouts, when scarring begins to form, or when acne significantly impacts your emotional well-being. A board-certified dermatologist can diagnose your specific acne type, prescribe targeted medications, and build a plan that actually matches your skin’s biology—not just generic advice from the internet.
Now let me break down each warning sign so you know exactly where you stand.
Sign #1: Over-the-Counter Products Have Stopped Working
I always tell people to give OTC acne treatments a fair shot. Benzoyl peroxide, salicylic acid, adapalene (Differin)—these are legitimate, evidence-backed ingredients. The American Academy of Dermatology recommends trying them consistently for at least two to three months before deciding they’ve failed.
But here’s the key word: consistently. If you’ve genuinely used a well-formulated beginner acne treatment for 12 weeks—same routine, every day, no skipping—and your skin hasn’t meaningfully improved? That’s your signal. OTC products have a ceiling. Prescription retinoids, oral antibiotics, and hormonal therapies operate on a completely different level. You’re not weak for needing them; you’re smart for recognizing when to escalate.
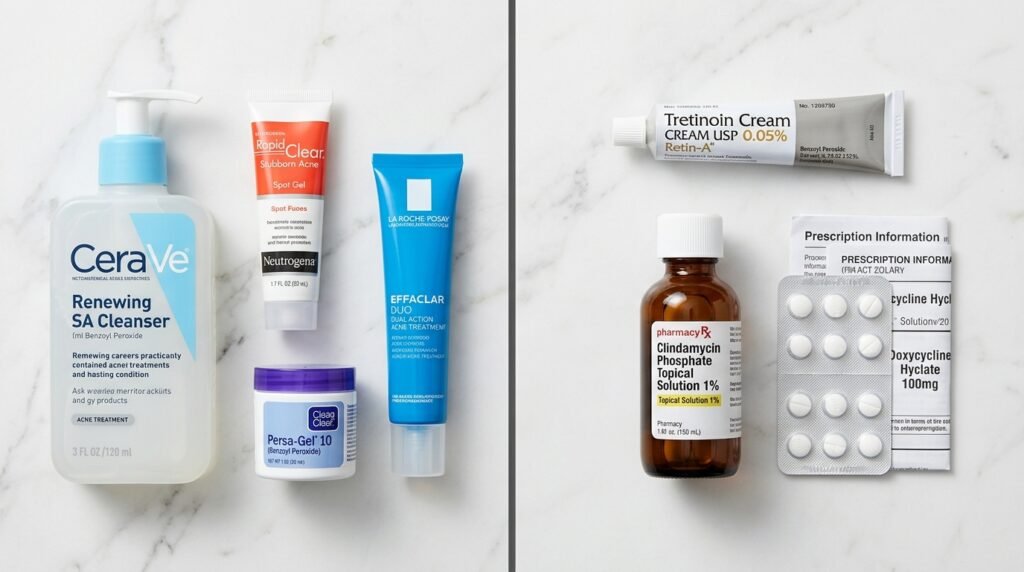
Sign #2: You’re Dealing with Cystic Acne
Let me be blunt: cystic acne is not something you should fight alone. Those deep, painful, under-the-skin bumps that feel like tiny volcanoes? They form when infection and inflammation penetrate deep into the dermis—far beyond where any face wash can reach. According to the National Institute of Arthritis and Musculoskeletal and Skin Diseases (NIAMS), cystic acne carries the highest risk of permanent scarring.
I’ve seen too many people try to “tough it out” with cystic breakouts, slathering on tea tree oil and praying. IMO, that’s like putting a Band-Aid on a broken bone. A dermatologist can offer cortisone injections that flatten a cyst within 24–48 hours, prescribe isotretinoin for chronic cases, or recommend combination therapies that attack the problem from multiple angles. If you’re unsure about what’s causing your acne at this level, professional diagnosis becomes non-negotiable.
Sign #3: Acne Scarring Is Getting Worse
This one hits hard because acne scarring is often irreversible without professional intervention. Every inflamed breakout you leave untreated is rolling the dice on a permanent mark. Ice pick scars, boxcar scars, rolling scars, post-inflammatory hyperpigmentation—once these set in, no drugstore cream will erase them.
Here’s my myth-bust for you: Vitamin C serums and niacinamide can help fade dark marks (post-inflammatory hyperpigmentation), but they cannot rebuild collagen in a true atrophic scar. That requires professional procedures—microneedling, chemical peels, fractional laser, or subcision. If you notice your skin texture changing and old breakout sites aren’t smoothing out, get to a dermatologist for acne scarring assessment before the damage accumulates further. Early treatment can literally save your skin. Check out our guide on common skin concerns for more on this topic.
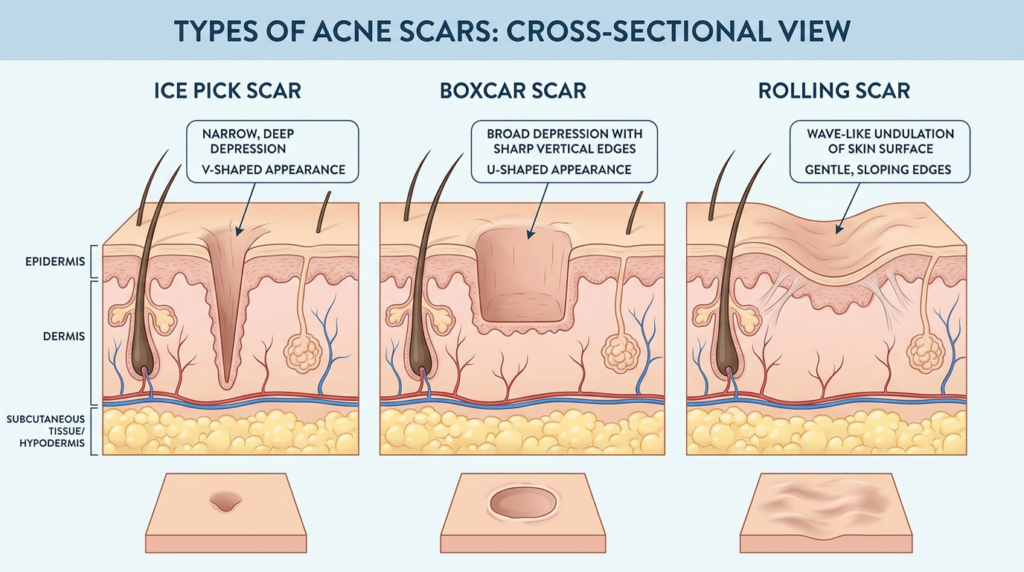
Sign #4: Your Acne Is Wrecking Your Mental Health
This is the sign people dismiss the most—and it might be the most important one. Research published in the Journal of the American Academy of Dermatology has repeatedly linked acne to higher rates of depression, anxiety, and social withdrawal. If you’re canceling plans, avoiding mirrors, or feeling genuinely distressed about your skin, that alone is reason enough to see a dermatologist.
You don’t need to hit some arbitrary “severity threshold.” Your skin doesn’t need to look like a textbook photo of severe acne to warrant professional care. A dermatologist treats the patient, not just the pimple count. Period.
Sign #5: You’re an Adult and Acne Won’t Quit
If you thought acne was something you’d leave behind with your high school yearbook, welcome to the club nobody wanted to join. Adult acne affects up to 15% of women and 5% of men, and it plays by different rules than teenage breakouts. It tends to cluster around the jawline and chin, often flares cyclically, and frequently has hormonal roots that OTC products simply can’t address.
I’ve talked to countless adults in their 30s and 40s who feel embarrassed even bringing it up—like they should have “grown out of it.” Nah. Adult acne is incredibly common, medically legitimate, and highly treatable with the right approach. If you’re just starting to explore your options, know that a dermatologist can run hormone panels, check for underlying conditions like PCOS, and prescribe targeted solutions that a general practitioner might overlook.
Sign #6: You Suspect a Hormonal Imbalance
Hormonal acne has some pretty distinctive fingerprints: breakouts that sync with your menstrual cycle, deep cysts along the jawline and lower face, and acne that started or worsened after stopping birth control, during pregnancy, or around perimenopause. If any of that sounds familiar, a dermatologist is your best ally.
Why? Because hormonal acne treatment often involves medications like spironolactone, certain oral contraceptives, or other androgen blockers—all of which require a prescription and medical monitoring. No amount of routine optimization will override an internal hormonal driver. You need someone who can look under the hood, not just wax the car. 🙂
Sign #7: You’ve Developed Sudden, Severe Acne
If your skin went from relatively clear to full-blown severe acne seemingly overnight, don’t brush it off. Sudden onset acne can signal medication side effects, hormonal disorders, or even underlying health conditions that need investigation. The Mayo Clinic notes that certain medications—lithium, corticosteroids, androgens, and some anticonvulsants—can trigger acute breakouts.
I’ve personally seen cases where sudden severe acne was the first visible symptom of a hormonal tumor. Rare? Yes. Worth investigating? Absolutely. When acne appears out of nowhere with unusual intensity, a dermatologist won’t just treat the surface—they’ll dig into the why. And that’s the kind of care a face wash will never provide.

What to Expect at Your First Dermatology Appointment
Walking into a dermatologist’s office for the first time can feel weirdly intimidating—but honestly, it shouldn’t. Here’s a quick rundown of what typically happens:
- Medical history review: They’ll ask about your skincare routine, past treatments, medications, family history, and menstrual cycle (if applicable).
- Skin examination: The dermatologist will assess your acne type, severity, and any existing scarring. They may use a dermatoscope or Wood’s lamp.
- Treatment plan: Expect a customized plan—this could range from topical prescriptions to oral medications to in-office procedures, depending on your situation.
- Follow-up schedule: Most dermatologists schedule a follow-up in 6–8 weeks to evaluate progress and adjust the plan.
Pro tip from someone who’s been through it: Bring a list of every product and medication you’ve tried, including how long you used each one. This saves time and helps your dermatologist avoid recommending something you’ve already failed on. For a full breakdown of treatment categories, browse our acne treatments guide.
Frequently Asked Questions
How bad does acne have to be to see a dermatologist?
It doesn’t need to be “bad” at all. If over-the-counter products haven’t improved your skin after 8–12 weeks, you’re developing scars, or your acne affects your confidence and mental health, you have every reason to book an appointment. Dermatologists treat mild acne too—and early intervention often prevents escalation.
Can a dermatologist cure acne permanently?
A permanent cure isn’t always guaranteed, but treatments like isotretinoin (Accutane) produce long-term remission in a significant percentage of patients. Hormonal therapies and tailored prescription regimens can also manage acne effectively for years. Your dermatologist will set realistic expectations based on your specific case.
What will a dermatologist prescribe for acne on the first visit?
For mild-to-moderate acne, expect topical retinoids (like tretinoin), benzoyl peroxide, or topical antibiotics. For more severe presentations, they may start oral antibiotics, hormonal therapy like spironolactone, or open a discussion about isotretinoin. Every plan gets tailored to your skin, history, and goals.
Is it worth seeing a dermatologist for mild acne?
100% yes. A dermatologist identifies your specific acne type, recommends prescription-strength products that outperform OTC options, and helps you avoid scarring before it starts. Think of it as an investment—early, targeted treatment almost always beats years of trial-and-error guesswork. TBH, I wish I’d gone sooner myself.
My Top Recommended Gear
While nothing replaces professional dermatological care, these are the products I consistently recommend to complement a prescription acne treatment plan. They’re well-formulated, affordable, and backed by solid clinical data:
- CeraVe Acne Foaming Cream Cleanser (4% Benzoyl Peroxide): The gold standard gentle BP cleanser that dermatologists love. Check price on Amazon
- La Roche-Posay Effaclar Adapalene Gel 0.1% (Differin Generic): The strongest OTC retinoid available—perfect as a bridge before or alongside prescription treatments. Check price on Amazon
- EltaMD UV Clear Broad-Spectrum SPF 46: A non-comedogenic sunscreen designed for acne-prone skin. Essential when using retinoids or post-procedure. Check price on Amazon
Disclaimer: This post contains affiliate links. As an Amazon Associate and ClickBank Partner, I may earn a commission from qualifying purchases at no additional cost to you.







